WHITE and Numb Fingertips
In sensitive individuals, after brief exposure to cold (within seconds) or during stress, one or more fingertips on one or both sides become pale and numb and then blue and then red; the attack may last from several minutes to hours (Raynaud’s phenomenon or syndrome).
Repeated use of vibration tools, such as hammer jack, may cause vibration white finger or hand-arm vibration syndrome (HAVS) with occasional numbness in the fingertips, which may become permanent with time. Fingertip discoloration does not occur during vibration but after exposure to cold or stress (Raynaud’s phenomenon–see above) 1.
Within 24 hours of using the hand as a hammer, the 3rd, 4th and 5th finger (or only one or two of them) and related part of the palm may suddenly become white or bluish, numb, cold and painful due to damage of the ulnar artery and nerve; the condition, which is known as hypothenar hand syndrome, may eventually improve; cold sensitivity may persist 2.
Frostnip. After prolonged exposure (minutes to hours) to cold, the hands and fingers may become cold, pale, bluish (cyanotic), stiff and, possibly, numb and tingly; reheating may trigger annoying pain in the nail beds 3.
Second-degree frostbite. After prolonged exposure to severe cold (hours, but can be minutes), the fingertips may become firm (“wooden”), waxy white, with eventual blisters developing 12-24 hours after the cold exposure; there is a loss of sensation for touch and, to some extent, for pain 6.
Third-degree burn or scald. After contact with hot objects, water vapors, the fingertips may become white with a leathery appearance and transient or permanent loss of sensation to touch and pain 4.
In arterial embolism, one or more fingers suddenly become cold, pale or blue, painful, weak, numb or tingly. Cramps may appear and the finger may be hard to move. If not treated promptly, ulcers or gangrene can develop 5.
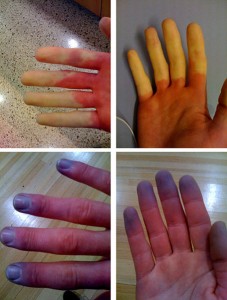
Picture 1. Raynaud phenomenon
First phase of the attack: white fingers
Second phase: blue fingers
(source: Wikimedia, CC license)
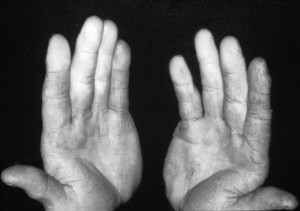
Picture 2. Vibration white finger
due to working with hammer jack
(source: cdc.gov, Public Domain)
RED Fingertips
Contact with the stinging nettle leaves or stems usually causes burning, itchy, red patches (hives, urticaria); numbness may persist for more than 12 hours 7,8.
In sensitive people, contact with poison ivy, oak or sumac can cause an allergic reaction with red, burning, itchy and swollen skin; numbness and tingling may persist for several hours 9,10.
Deep second-degree burn or scald. After contact with a hot object, liquid or vapors, the affected fingertips are usually red and tender, but can later become more or less numb and remain so for up to a month 11,12.
Chilblains (pernio). In sensitive people, exposure of the fingers to nonfreezing temperatures below 60 °F (60 °C) and subsequent reheating may result in red or violaceous, blistering, itchy, tingly and numb fingertips or toes. Numbness usually goes away in one to three weeks or may persist for years 6,13.
A minor cut or puncture of the fingertip can result in felon or staphylococcal whitlow — an infection with red, swollen, painful and, eventually, numb fingertip pulp 14,15.
Stings of the venomous insects, such as a bee, wasp, hornet, spider (black widow, brown recluse spider) and scorpion, can cause burning pain, redness, blisters and swelling in the affected fingertip, followed by tingling and numbness, which may persist for a day or two 16,17,18.
Bites of non-venomous insects, such as a mosquito, horse fly, flea, scabies mites, bed bugs, lice, ticks, chiggers and cockroaches, can cause itchy red bumps, sometimes followed by tingling and numbness 19. NOTE: The exact site of the insect bite may not always be seen.
Bites of venomous snakes, such as cobra or rattlesnake, to the arm can cause numbness and tingling in the affected area spreading toward the fingertips 20.
Vasculitis:
- In rheumatoid vasculitis (in rheumatoid arthritis and systemic lupus erythematosus or SLE), numbness and pits in the fingertips and red sores around the nails may develop 21,22.
- Symptoms of Churg-Strauss syndrome may include difficulty breathing (asthma), and red-bluish and numb fingertips 23.
One side effect of certain chemotherapeutics is hand-foot syndrome (acral erythema or palmar-plantar erythrodysesthesia) with numbness, tingling, pain, redness, swelling or flaking of the palms, fingers, soles and toes.
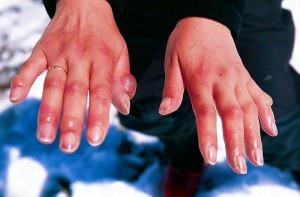
Picture 3. Chilblains
Red, swollen fingertips with big blisters
(source: Wikimedia, CC license)
PINK Fingers
Poisoning with elemental (metal) mercury in children: pink, numb or painful fingers, peeling hands and leg cramps (acrodynia) 24.
BLUE or PURPLE Fingertips
After an injury, for example, with a hammer, the affected fingertip usually becomes tender and bruised: red, then swollen and partially numb then dark blue-purple and then yellow-green.
Achenbach syndrome (paroxysmal hand hematoma, finger apoplexy) 25 consists of sudden pain, itching, stinging, swelling, coolness, bruising and, sometimes, numbness on the palmar side of one or, rarely, more fingers that last for few days and then resolve spontaneously. This benign condition is due to spontaneous bleeding in the finger. Triggers include physical work with hands, minor trauma, exposure to cold.
The affected individuals often have Raynaud’s phenomenon, migraine, chronic venous insufficiency (varicose veins), gallbladder disease, allergies or a blood disorder, such as anemia or thrombophilia. The condition may run in families. Blood and other tests are usually normal.
Peripheral Cyanosis
Cyanosis means bluish discoloration of the skin due to lack of oxygen in the tissues.
In peripheral cyanosis, fingers and toes, especially nail beds, and, sometimes, the skin around the mouth, but NOT lips and tongue, become bluish 26.
Peripheral cyanosis is caused by impaired circulation in the limbs.
Acute (sudden) peripheral cyanosis can be caused by 26:
- Cold injuries:
- Hypothermia due to prolonged immersion in cold water or exposure to cold air 27,29
- Chilblains 28
- Deep frostbite (persistent cyanosis and numbness after rewarming are bad prognostic signs) 30
- Raynaud’s phenomenon–see above under white fingertips
- Prolonged seizures (tonic-clonic seizures or grand mal epilepsy) 32
- Acute artery narrowing due to an embolus (due to atrial fibrillation, thoracic outlet syndrome) or crush injury (sudden pain, and cool, pale and, later, blue-purple fingers) 33
- Hypovolemic shock (due to severe dehydration, bleeding or diarrhea) or cardiogenic shock (due to heart attack, arrhythmia)
- Pheochromocytoma: cyanosis and tingling in the fingertips, finger tremor, pale skin, anxiety, high blood pressure 34
- Drugs: beta-blockers, methysergide, ergotamine, epinephrine and other drugs can increase the risk of Raynaud’s phenomenon with white, blue and red fingertips 35.
Some individuals experience sudden blue discoloration, coolness, swelling, pain (not always), numbness or “pins and needles” in one or more fingers without apparent reason. This is called “acute blue finger” or “blue finger syndrome” 31. Symptoms may last for few days and rarely recur. Possible risk factors include smoking, atherosclerosis, Raynaud’s phenomenon, trauma, frostbite, thoracic outlet syndrome, cryoglobulinemia and polycythemia. The condition is often benign, and the risk of thrombosis or embolism is low.
Chronic (persistent) peripheral cyanosis may be caused by 36:
- Atherosclerosis, mainly in older smokers and diabetics and those with high blood pressure and high blood cholesterol
- Venous thoracic outlet syndrome
- Vasculitis, for example, Buerger’s disease 39 and rheumatoid vasculitis 40
- Cryoglobulinemia (abnormal blood proteins causing blood clotting), for example, in hepatitis C 41
- Congestive heart failure
- Deep vein thrombosis or arterial thrombosis 42
Acrocyanosis is persistent bluish-purple discoloration of the fingertips (and sometimes, hands, feet, knees, nose, lips and nipples). Cyanosis is aggravated by cold or stress or by hanging hands down. There are no attacks, and cyanosis persists after rewarming. Other symptoms may include numbness in the fingertips and cool and sweaty palms. This benign condition, which tends to improve with time, is frequently seen in young women with anorexia nervosa; other causes include ovarian cancer, Hodgkin lymphoma, cryoglobulinemia, hypoxemia low oxygenation of the blood) 38. The risk of arterial occlusion or skin ulcers is not increased. In newborns, acrocyanosis is usually caused by metabolic disorders.
Central Cyanosis
In central cyanosis, hands and feet, especially nail beds, lips, gums and tongue have bluish discoloration but are not cold (unless the causes of peripheral cyanosis are present) 26.
Central cyanosis is caused by decreased oxygenation of the blood:
Acute (sudden) central cyanosis 26:
- Lack of oxygen in the air (hypoxia) in high altitudes (climbers, pilots) 43
- Respiratory disorders: croup, whooping cough (pertussis), epiglottitis, bronchiolitis, severe attack of asthma, aspiration of vomitus, severe pneumonia, pulmonary edema, pulmonary embolism, tension pneumothorax, acute respiratory distress syndrome (ARDS)
- Heart disorders: heart attack, arrhythmia
- Methemoglobinemia: ingestion of or skin exposure to aniline, benzocaine, dapsone, pyridium, nitrites, nitrates, naphthalene, primaquine
- Sulfhemoglobinemia: an overdose of certain drugs (acetanilide, metoclopramide, nitrates, phenacetin, phenazopyridine, sulfasalazine, sulfonamides), ingestion of household cleansers (hydroxylamine sulfate) 26,44
- Disseminated intravascular coagulation (DIC), for example, in sepsis (see more causes below under Gangrene)
- Poisoning: solvents (chlorobenzene), pesticides (arsenic, strychnine, organophosphates) 45
Chronic (persistent) central cyanosis 26:
- Heart disorders: congenital disorders, cardiomyopathy, heart valve disease (infectious endocarditis, rheumatic fever, hypertension, aortic aneurysm) 42
- Respiratory disorders: chronic obstructive pulmonary disease or COPD (bronchitis, emphysema), bronchiectasis, pulmonary fibrosis, cystic fibrosis
- Severe anemia
- Blood hyperviscosity: Waldenström macroglobulinemia, polycythemia vera, multiple myeloma, leukemia, thrombocythemia, paraneoplastic syndrome in certain cancers 47
- Obstructive sleep apnea
- Genetic methemoglobinemia
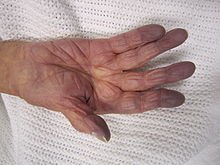
Picture 4. Cyanosis
Blue fingertips and hand due to lack of oxygen in the blood
(source: Wikimedia, CC license)
BLACK Fingertips
In the third-degree frostbite, the affected fingertips become bluish-greyish or black and numb; superficial layers may peel off. Ulcers and an eventual permanent decrease of the fingertip sensitivity may develop 6,13.
In the fourth-degree frostbite, gangrene (tissue death) can occur, especially after freeze-thaw-refreeze situation 6,13.
In the fourth-degree burn, the fingertips carbonize and eventually crumble and fall off 4.
Dry Gangrene
Gangrene means tissue death (necrosis); it is caused by blocked circulation, bacterial infection or trauma 48.
Dry gangrene can develop in severe atherosclerosis (in diabetes), vasculitis (for example, in Buerger’s disease), scleroderma or severe Raynaud’s disease 49.
Symptoms of dry gangrene: the affected fingertip becomes red, then pale, cold and numb, then brown, purple or black, it shrivels up and eventually fall off 48,51.
Wet Gangrene
Wet gangrene can occur due to bacterial infection in severe frostbite, burn or injury.
Symptoms of wet gangrene: painful, swollen fingertips with foul-smelling discharge; the fingertips crumbles and eventually falls off (autoamputation) 48,51.
ACUTE gangrene of the fingertips 49,50:
- Tight wound dressing or splint immobilization of the finger 52
- Fourth-degree frostbite 6,13, third- and fourth-degree burn 4, electrical injury 53, irradiation injury (>5,000 rads)
- Severe injury to the finger, hand or arm 55, a cut of radial artery 56
- Artery occlusion after surgical artery ligation, a complication of surgery wound infection 57
- Infections: felon (cellulitis of the fingertip) 58, cellulitis of the hand, necrotizing fasciitis 59
- Prolonged contact with caustic potash, nitric, or sulfuric acid, spilling of diluted (1%) phenol (carbolic acid) solution over the skin 61
- Blood clot (thrombus) in deep venous thrombosis 62,63
- Hypersensitivity angiitis 50
- Necrotizing vasculitis: rheumatoid vasculitis, polyarteritis nodosa, Buerger’s disease 39
- Plague 64
- Disseminated intravascular coagulation (DIC) due to sepsis, leukemia, malaria, viral gastroenteritis, snake bites, transfusion reactions, recreational drugs, etc. with symmetrical peripheral gangrene affecting the fingertips and toes on both sides 65,66,67,68
- Gangrenous ergotism (the drug ergotamine, rarely: infected rye bread) 69,70
- A complication of chemotherapy (for example, the combination of bleomycin and methotrexate) 71
- Warfarin-induced skin necrosis 72
Picture 5. Gangrene of the fingertips in plague due to sepsis
(source: cdc.gov)
CHRONIC causes of gangrene of the fingertips 49,50:
- Hyperglycemia in long-term, poorly controlled diabetes 1 or 2
- Arteriosclerosis (in older people, smokers, those with high cholesterol), eventually complicated by emboli lodged in the finger arteries 42
- Vasculitis: polyarteritis nodosa 73, Churg-Strauss syndrome (allergic vasculitis) 23,74, microscopic polyangiitis 75, rheumatoid vasculitis (SLE, rheumatoid arthritis) 76, Buerger’s disease (in heavy smokers) 39
- Hypereosinophilic syndrome 77
- Severe Raynaud’s phenomenon associated with scleroderma (CREST syndrome) or lupus 50,60
- Chronic disseminated intravascular coagulation (DIC) as a complication of ulcerative colitis, Crohn’s disease, leukemia, cancer, sarcoidosis, retained dead fetus syndrome 46
- Cryoglobulinemia, for example, in hepatitis C 41
- Antiphospholipid syndrome (APS), which may be associated with systemic lupus erythematosus (SLE) or other rheumatic diseases 37
- Thrombotic thrombocytopenic purpura (TTP) 72
- References
- Patient.info (Hand-arm vibration syndrome)
- PMC (Hypothenar hammer hand syndrome)
- Emedicine (Frostbite)
- Mayo Clinic (Burn injury)
- Angiologist.com (Embolism in the upper extremity)
- Armypubs.army.mil (Cold injuries)
- Ucdavis.edu (Stinging nettle)
- Oardc.ohio-state.edu (Stinging nettle)
- Aad.org (Poison ivy, oak and sumac)
- Poison-ivy.org (Poison oak)
- Regionshospital.com (Pins and needles after a burn injury)
- Burns: Regenerative Medicine and Therapy, y.2004 (p.21) (Burns)
- Army.mil (Cold injuries)
- Bupa.co.uk (Felon complications)
- Drugs.com (Felon)
- MedlinePlus (Insect bites)
- MedlinePlus (Insect bites first aid)
- WebMD (Insect bites)
- Dermnetnz.org (Insect bites and stings)
- MedlinePlus (Snake bites)
- Clevelandclinic.org (Rheumatoid vasculitis)
- Nhlbi.nih.gov (Vasculitis)
- PMC (Churg-Strauss syndrome)
- EPA.gov (Mercury poisoning)
- Kampfen S et al, 2005, A Painful Blue Thumb: A Case of Achenbach’s Syndrome ScienceDirect
- Patient.info (Central and peripheral cyanosis)
- Wisc.edu (Cryoglobulinemia and acral cyanosis)
- Wiley.com (Primary amyloidosis and Raynaud’s phenomenon)
- Rosen’s Emergency Medicine: Concepts and Clinical Practice, 7th edition, y.2009, Volume 1 (p.1873) (Hypothermia)
- Emedicine (Frostbite)
- PMC (The acute blue finger)
- Devinski O, 2004, Effects of Seizures on Autonomic and Cardiovascular Function PubMed Central
- Practicalplasticsurgery.org (Crush injury)
- Healthlinkbc.ca (Pheochromocytoma)
- Japi.org (Antiphospholipid syndrome and Raynaud’s phenomenon)
- Vascularweb.org (Arm artery disease)
- PubMed (Antiphospholipid syndrome)
- Das S et al, 2013, Acrocyanosis: An Overview PubMed Central
- Emedicine (Buerger’s disease)
- Clevelandclinic.org (Rheumatoid vasculitis)
- Emedicine (Cryoglobulinemia)
- PubMed (Acute purple digits)
- Dedicated559.com (Hypoxia)
- PMC (Cleansers (hydroxylamine sulfate)
- Thebestcontrol.com (Strychnine, arsenic poisoning)
- Emedicine (Disseminated intravascular coagulation (DIC))
- Emedicine (Hyperviscosity syndrome)
- NHS.uk (Gangrene)
- Patient.info (Gangrene cause)
- PMC (Causes of gangrene)
- NHS.uk (Gangrene development)
- Acep.org (Tight wound dressing)
- Emedicine (Electrical burns)
- NIH.gov/books (Dissection of the thoracic aorta)
- PMC (Acute compartment syndrome of the forearm and hand)
- PubMed (A cut of radial artery)
- Oxfordjournals.org (Surgical wound infection)
- Bupa.co.uk (Felon complications)
- Emedicine (Necrotizing fasciitis)
- Mayo Clinic (Raynaud’s disease complications)
- Phenol first aid and PPE Cornell University
- PubMed (Gangrenous fingers)
- Natfonline.org (Deep venous thrombosis)
- Uiowa.edu (Gangrene in plague)
- PubMed (Venous thrombosis)
- PMC (Symetrical peripheral gangrene and disseminated intravascular coagulation)
- PubMed (Malaria)
- Emedicine (Disseminated intravascular coagulation)
- Drugs.com (Ergotamine)
- FPnotebook.com (Ergotism)
- PubMed (Chemotherapy)
- Orionwellspring.com (Blue toes and fingers)
- Emedicine (Polyarteritis nodosa)
- Mja.com.au (Churg-Strauss syndrome)
- Hopkinsvasculitis.org (Microscopic polyangiitis)
- Rheumatology.org (Gangrene of a finger in rheumatoid arthritis – picture)
- Jst.go.jp (Hypereosinophilic syndrome)



Snakes are venomous not poisonous
My thimb middle and forefinger has mild itch cramp may be doe to stress of continosly removing lice and nits it is sometimes bluish what is the treatment it is now 10 days i wake up with pain and cramps
If the fingers are bluish, it can be a problem with circulation within them, so I suggest you to visit a doctor.
Atfer a herion I.V hit (knowing only a couple weeks earlie on a absisis what I had to go A.E did not stay for outcome)it got better.
then fastfored two weeks done it again but this time its been wried my hand is not right its scaring me.
it started with non.stop pins niddles then small finger wnt spas on me then the one next to it now its painfull very hot feels like its stuck now its blue and feels like getting wrost what do I do?
Go to the emergency room as soon as possible.
Hi,4days back i suddenly noticed my thumb n index finger the tip portion red and the middle finger tip and middle portion red..no pain, no nothing..after 2hrs it disappeared…again same thing today..only these 3 fingers…pls advise….
Would you say it was triggered by stress or cold? Such color change can be a part of Raynaud’s phenomenon.
I was watching a movie one evening about three weeks ago. It had been a tired day so I rested a lot (I have Lupus, Fibro, Diabetes, and a number of other things). Out of nowhere, this pain ravaged the thumb edge of my pointer finger. Right before my eyes there formed a whiteness about the size of a dime. The pain lasted for just over two hours then stopped as suddenly as it started. I was a total sweat mess from it. I couldn’t do anything because of this pain. The whiteness was late by late the next day. This has only happened once but I thought I’d ask you about it.
With conditions, listed, I think you are at increased risk of Raynaud’s phenomenon, when such finger pain and whiteness can happen, but usually in more fingers.
But this could also happen due to a blood clot in a finger, for example. You may want to read this:
http://www.ehealthstar.com/what-causes-numb-and-white-blue-red-pink-or-black-fingers.php
A couple days ago I hit my Palm on something. The next day my pinky finger was numb and very cold. Then the next day while dealing with an uncomfortable pinky all of a sudden my ring finger went numb and it has now been 6 hours and has not got better. Plus my nail bed and the top behind is a blueish purple color. The rest of my finger looks fine. Don’t know what’s going on and kind of scared cuz I can’t feel the top of the finger. What could it be and what should I do.
I’m late to this but go to a doctor. It could be a nerve or artery injury, which can leave a permanent damage if you do not treat it.
Last month my father suffered from cold fingers with bluish colour ring finger. but after few days it is now cured totally . the bluish & blackish surface of finger turned to normal new skin colour. The only thing is the ring finger remains cold sometimes.
He may want to have some investigations done to find the underlying cause, because this may repeat and can be potentially harmful for the fingers.
My mom right hand ring finger and left hands index finger has become blue since 10-15 days now. Visited 3 doctors and they said it may be clot and poor blood circulation, but the prescribed medicine did not cure or relieve her from pain. She mentions she feel acute pain at moments and unable to hold anything. She is currently on the following medicines Complamila (twice a day), Livogel and Thrombofob gel.
She is diabetic but normally its in control, she had also got the test done a month back and the Diabetes Specialist also diagnosed the fingers as blood clot.
After reading the above article, I’m quite tensed and would like an advised if I should take her for further more check ups because the problem has not subsided even after treatment of 15 days or more now.
Yes, I strongly suggest you to take her to more investigations as soon as possible, because blood clots (if it turns out this is the cause) can be life threatening.
whenever i deal with cold water my finger tips become pail with pain on these tips. can you please tell me its cause. whether it is some kind of disease. if it is then please tell me how it canbe corrected
One possible cause is Raynaud’s disease, which does not have a known cause. When the cause is known it is called Raynaud’s phenomenon. A doctor can tell you what is a cause and what you can do.
All the toes in my left foot are numb, particularly underneath, accompanied with a sharp stinging pain. They are white compared to the toes on my right foot which are more of a pinkish color. Also the middle of my foot feels as if it is tight, almost like a cramp. No recent trauma. Went to see a dr this morning and he said he thought I slept with my foot balled up. I’m starting t think it’s something else. Please help.
If it were just sleeping with a bent foot, the white color would not persist. I strongly suggest you to visit a doctor again to exclude the possibility of a blocked artery or a nerve damage. The fingers become white when there is no blood in them. You may also want to make few photos of both of your feet in case the white color disappears before you see a doctor.
Off and on for the past week, seemingly when I’ve ran errands or driving home after work in a cold car, my right middle finger tip (from last finger joint to to tip) has suddenly become tingly and numb..feels like it’s been asleep. Lasts anywhere from 30 minutes to an hour. During that time that it’s tingling and numb, the underside of my finger in the middle section just below the numbness is blue-purplish in color like a bruise. Later when my hands are thoroughly warm and the sensation subsides… the bruising color on my skin also goes away. I live in Tennessee and the weather has been only mildly cold lately. It hasn’t been below 30 degrees this week and I’m not out in this temperature but for 5-10 minutes when this begins. What could this be and is it something to be concerned with?
Tracy, you may want to visit a doctor to get an exact diagnosis. Possible causes may include an embolus in the artery of the middle finger, Raynaud’s phenomenon, “blue finger syndrome”…
Had a very bad cold for over a week now which is nothing new but I’m starting to get pins and needles in my right thumb and the whole thumb turns white ( very pale ) didn’t think nothing of it at first but this happens quite a few times now , went doctors for my cold and the thumb went again in front of the doctor who said it was strange but did nothing , what the hell could this be ?
Mark, if this will continue I suggest you to insist in getting the exact diagnosis. The white color is obviously related to a circulation problem, such as Raynaud’s phenomenon or an embolus, for example.
My husband fell and injured his elbow.he may have tore or broke it. His hands are swollen and fingers are turning blue. Je doesnt want to see his doctor because hes a stroke patient and doesnt want his doctor to know he drinks or does cocaine.why are his finger blue?
Rebecca, this sounds as an urgent medical condition to me. If he does not get treatment soon, he may lose the fingers. The fingers can be blue because they do not get enough blood.
Dear Sir,
I have got servere pain on my thumb tip and can see blue colour on the tip. Kindly guide vme what could it be and any treatment or precautions I can take.
Thanks for your co-operation.
Hi. If it is diffuse and permanent bluish discoloration lasting for more than few days, it’s probably due to impaired blood flow, which is usually caused by atherosclerosis or a clot lodged in the thumb artery. I strongly recommend you to visit a doctor to get correct diagnosis and treatment. So, if it is impaired blood flow, it is not likely you will be able to cure it by yourself by some sort of remedy.