What is shingles?
Shingles or herpes zoster is a localized painful rash caused by a reactivation of the chickenpox (Varicella-zoster) virus in your body [6].
Symptoms and Signs
Early symptoms
For 1-10 days before the rash outbreak, you may experience [4,6]:
- Malaise, headache, fatigue or, rarely, fever
- Severe burning pain, tingling, numbness or itch in one body region
- Swollen lymph nodes in the neck, armpit or groin on the same side
The rash stage
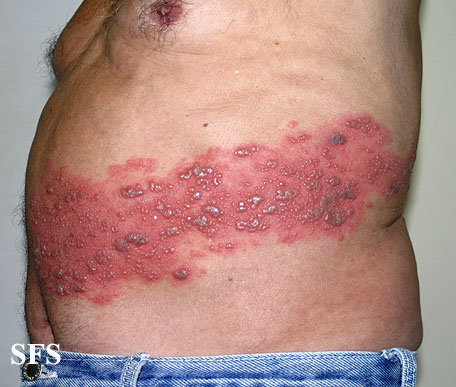
Few days after onset of pain, a red rash develops in a band-like pattern on one side of the body, most commonly on the trunk, neck or around the eye, but sometimes on the scalp, in the ears, nose or mouth, on the palms, buttocks or genitals (Pictures 1,2) [2,6].
Picture 1. Shingles with a band-like pattern
limited to one side of the body
(source: SF da Silva, MD, Dermatology Atlas)
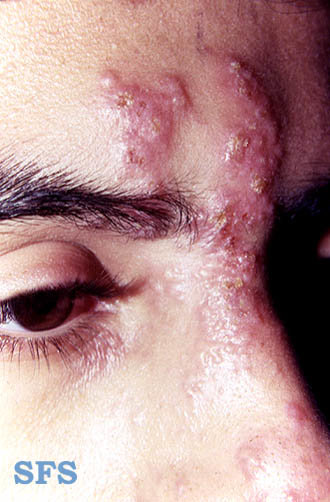
Picture 2. Shingles on one side of
the forehead and nose
(source: SF da Silva, MD, Dermatology Atlas)
The rash develops in the following phases [4,5]:
- Red patches, spots or bumps (erythema, macules or papules)
- Blisters with clear fluid (vesicles)
- Blisters with cloudy fluid (pustules)
- Ulcers
- Crusts
The crusts fall off spontaneously within 2-4 weeks [4]. The pain can disappear along with the rash or can persist for several weeks or months [4].
Atypical shingles
Mainly in children, shingles can appear with rash and no pain, or pain and no rash [2,7].
In individuals with poor immunity, shingles can appear on both sides of the body (bilateral shingles), involve large areas of the skin and internal organs (disseminated shingles) or recur several times (recurrent shingles) [4,7].
How does shingles develop?
When you have chickenpox, some viruses can enter the nerves in the skin and remain dormant (silent) in the nerve roots near the spinal cord. Years or decades later, a triggering event, such as stress or disease, can reactivate the viruses, which results in shingles [6].
Who can get shingles?
Anyone who has had chickenpox (even if passed unnoticed) or received varicella vaccine can get shingles [9].
- About 30% of adults, especially those after the age of 50, get shingles once in their lifetime [8].
- Children and young adults rarely get shingles [6].
You cannot get shingles if you previously have not had chickenpox or received varicella vaccine [9].
Can shingles spread to other parts of the body by touch?
Probably not.
Can you get shingles more than once?
Up to about 6% of people can get shingles twice or more times [2,21].
Risk Factors
Risk factors for shingles include [5,19,20,35]:
- Old age
- Genetic predisposition
- Having chickenpox before 18 months of age
- Poor immunity (in HIV/AIDS, blood cancer, such as lymphoma or leukemia, long-term treatment with steroids, chemotherapy or immunosuppressant therapy after organ transplantation
- Diabetes mellitus type 1
- Chronic lung or kidney disease
- An autoimmune disease (rheumatoid arthritis, systemic lupus erythematosus or inflammatory bowel disease: Chron’s disease or ulcerative colitis)
Triggers of shingles include [2,34,35]:
- Psychological stress, lack of sleep, depression or sexual abuse
- Physical trauma, an infection, herniated disc in the spine or spinal surgery
Is shingles contagious and how is it transmitted?
Shingles is contagious but cannot be transmitted directly from one person to another. You can contract the virus from someone who has shingles in the blistering phase, but only if you have never had chickenpox or received varicella vaccine [1]. After contracting the virus, you can develop chickenpox, not shingles [7]. Once you have chickenpox, you can develop shingles later in life, though.
The transmission of the virus is by a direct skin-to-skin contact or by sharing towels or gym equipment, for example [29].
The Herpes zoster virus probably does not spread by air (coughing, sneezing), so it is not likely you will contract it by just being in the same room with a person with shingles [12]. An airborne transmission may occur between a person with widespread shingles and a person with impaired immunity, though [10].
A pregnant woman who gets chickenpox 21-5 days before giving birth can pass the virus to the unborn baby who can then, in infancy or early childhood, develop shingles [6,13]. On the other hand, a pregnant woman with shingles will unlikely pass the virus to the unborn baby [33].
Shingles is not related to seasons and does not occur in epidemics [22].
Diagnosis
A doctor can usually recognize shingles from your medical history and a physical examination. Various tests can be used in unclear cases.
Blood tests:
- Varicella-zoster-specific IgM antibodies
Tests of the fluid from blisters (in decreasing order of sensitivity) [5,6]:
- Polymerase chain reaction (PCR) testing
- Direct fluorescent antibody (DFA) testing
- Tzanck smear
Chart 1. Conditions Similar to Shingles |
|
| Pain AND rash | Pain WITHOUT rash |
|
|
Chart 1 references: 11
Treatment
Home remedies, lotions and creams
The rash in the blistering phase should be covered by a wet non-occlusive dressing with aluminum acetate (Burow’s solution) for 30-60 minutes few times a day to reduce itch and the spread of the infection [14,25]. Dressing with petroleum jelly may better protect the rash against bacterial infections [2].
Applying an ice pack or cold, wet cloth for 10-15 minutes several times a day or having a cool bath or colloidal oatmeal bath may temporarily reduce the pain and itch [27].
There is INSUFFICIENT EVIDENCE about the effectiveness of lotions containing calamine [14] or menthol, antiseptic lotions [25], or creams containing capsaicin [36] or aspirin [20] in the reduction of pain and itch in shingles.
Do not apply any home-made paste (cornstarch, baking soda) on the rash, because it may increase the risk of an infection.
Antivirals
The antiviral drugs for shingles approved in the United States include acyclovir, valacyclovir and famciclovir. They are intended to treat moderate to severe pain and rash [26]. The individuals with normal immunity are usually treated by oral antivirals for 7 days and those with impaired immunity by oral or intravenous antivirals for up to 21 days.
The antiviral brivudin is approved in certain European countries [18].
Antivirals should always be used in older individuals and those with impaired immunity and when the ophthalmic nerve (around the eye) or large skin areas are affected [4].
The EFFECTS of antivirals:
- They decrease the severity and duration of symptoms [4].
- They are most effective when started within 72 hours of the rash onset; they can still help when started later but before the full crusting of all lesions [4,5,14,20].
- They only slightly decrease the risk of postherpetic neuralgia [16].
- Valacyclovir and famciclovir may be more effective than acyclovir [5,14,28,37].
- Topical antivirals (in creams) are not effective [5,26].
- Pregnant women should not take antivirals.
Analgesics
For mild pain [5,20,25]:
- Acetaminophen (paracetamol)
- Ibuprofen (can increase the risk of bacterial skin infections) [3]
- Aspirin (not for children and young adults, because it may trigger a severe liver and kidney damage – Reye’s, syndrome) [23]
- Tramadol
- Codeine
For moderate or severe acute pain, narcotics oxycodone or morphine can be used [5,20,26]. It is not clear if anticonvulsants gabapentin and pregabalin reduce acute pain, but they can reduce chronic pain [5,20,38].
Reducing pain by analgesics during the rash stage of shingles may decrease the risk of postherpetic neuralgia [4,5].
Antibiotics
Oral antibiotics are intended to treat secondary bacterial infection, which can develop in severe shingles [2]. Topical antibiotics should not be used [25].
Antihistamines
Antihistamines by mouth or as an ointment can help reduce severe itch [44].
Diet and supplements
There is no known diet to prevent or treat shingles [14].
While there is some weak evidence about the effectiveness of lysine supplements or foods with a high lysine/arginine ratio (milk, yogurt, cheese, papaya, beets) in the treatment of oral herpes (cold sores), there seems to be no such evidence for herpes zoster [30,31,39].
Some individuals with shingles have low blood vitamin C levels, but there is insufficient evidence about the effect of intravenous vitamin C on the reduction of chronic pain [24,32].
Even short-term moderate alcohol drinking can decrease immunity, so it reasonable to avoid alcohol during shingles [45].
Rest
When you have shingles, you usually do not need to rest in bed [14]. You should avoid activities that increase pain and those that allow the spread of the infection, such as visiting swimming pools and gym.
Therapies with insufficient evidence of effectiveness
There is INSUFFICIENT EVIDENCE about the effectiveness of the following treatments for pain or itch relief in shingles:
- Steroids (clobetasol, hydrocortisone, triamcinolone) [2,4,18,20]
- Acupuncture [41,42]
- Wet cupping [43]
- Zinc, colloidal silver, charcoal, table salt
- Herbs: apple cider vinegar, coconut oil, lavender oil, neem, oregano, eucalyptus
Prognosis and Complications
In young and otherwise healthy persons, shingles usually heal spontaneously and without complications within a month [6].
In elderly, the pain often persists for several months after the rash has cleared (postherpetic neuralgia). Deep shingles may leave permanent scars and pigmentations.
In up to 15% of the individuals with weak immunity, shingles that affect the brain (encephalitis), lungs (pneumonitis), liver (hepatitis) or other internal organs may result in death [6].
Localized complications [6,40]:
- Involvement of the ophthalmic nerve can result in temporary or permanent vision loss.
- Involvement of the facial and acoustic nerve can result in hearing loss, vertigo and partial paralysis of the face (Ramsay-Hunt syndrome).
- Damage to a sensory nerve can result in changed sensitivity, either decreased (numbness), increased (hyperesthesia) or unusual (allodynia).
- Damage to a motor nerve can result in muscle weakness or limb paralysis.
Herpes zoster increases the risk of heart attack and stroke in the first year of the symptoms onset [17].
Some individuals with severe shingles develop chronic fatigue syndrome, fibromyalgia or complex regional pain syndrome.
- References
- Shingles (herpes zoster) transmission CDC.gov
- Herpes zoster DermNetNZ
- Mikaeloff Y et al, 2008, Nonsteroidal anti-inflammatory drug use and the risk of severe skin and soft tissue complications in patients with varicella or zoster disease PubMed Central
- Gnann JW et al, 2002, Herpes zoster New England Journal of Medicine
- Fashner J et al, 2011, Herpes Zoster and Postherpetic Neuralgia: Prevention and Management
American Family Physician - Janniger CK, Herpes zoster, overview Emedicine
- Janniger CK, Herpes zoster, clinical presentation Emedicine
- Shingles (herpes zoster) overview CDC.gov
- Shingles (herpes zoster) clinical overview CDC.gov
- Preventing Varicella-Zoster Virus (VZV) Transmission from Zoster in Healthcare Settings CDC.gov
- Janniger CK, Herpes zoster, differential diagnosis Emedicine
- Protecting yourself from shingles MedlinePlus
- Shingles: Hope through research National Institute of Neurological Disorders and Stroke
- Janniger CK, Herpes zoster, treatment and management Emedicine
- Varicella zoster immune globulin, human (Rx) Medscape
- Chen N et al, 2014, Antiviral treatment for preventing nerve pain after shingles (postherpetic neuralgia) Cochrane
- Breuer J et al, 2014, Herpes zoster as a risk factor for stroke and TIA PubMed Central
- Wareham DW, 2007, Herpes zoster PubMed Central
- Kawai K et al, 2017, Risk Factors for Herpes Zoster: a Systematic Review and Meta-Analysis PubMed Central
- Cohen KR et al, 2013, Presentation and Management of Herpes Zoster (Shingles) in the Geriatric Population PubMed Central
- Kawai K et al, 2014 Systematic review of incidence and complications of herpes zoster: towards a global perspective BMJ Open
- Harpaz R et al, 2008, Prevention of Herpes Zoster; Recommendations of the Advisory Committee on Immunization Practices (ACIP) CDC.gov
- Shingles American Family Physician
- Schencking M et al, 2012, Intravenous Vitamin C in the treatment of shingles: Results of a multicenter prospective cohort study PubMed Central
- The diagnosis and management of herpes zoster and its complications bpac NZ
- Janniger CK, Herpes zoster, guidelines Emedicine
- 2015, Dermatologists share tips for treating shingles American Academy of Dermatology
- Bruxelle J et al, 2012, Effectiveness of antiviral treatment on acute phase of herpes zoster and development of post herpetic neuralgia: Review of international publications ScienceDirect
- 2016, Management of Varicella zoster virus (VZV) infections Federal Buerau of Prisons
- Gunn D, 2016, Varicella-Zoster Vaccine and Herpes Simplex Virus: Is There Cross Immunity? Proceedings of UCLA Healthcare
- Lysine uses WebMD
- Kapoor S, 2012, Vitamin C for attenuating postherpetic neuralgia pain: an emerging treatment alternative PubMed Central
- Pupco A et al, 2011, Herpes zoster during pregnancy PubMed Central
- Sansone RA et al, 2014, Herpes Zoster and Postherpetic Neuralgia: An Examination of Psychological Antecedents PubMed Central
- Baum SG, 2014, Shingles risk factors NEJM Journal Watch
- Yong LY et al, 2016, The Effectiveness and Safety of Topical Capsaicin in Postherpetic Neuralgia: A Systematic Review and Meta-analysis PubMed Central
- McDonald EM et al, 2012, Antivirals for management of herpes zoster including ophthalmicus: a systematic review of high-quality randomized controlled trials PubMed
- Berry JD et al, 2005, A single dose of gabapentin reduces acute pain and allodynia in patients with herpes zoster PubMed
- Walsh DE et al, 1983, Subjective response to lysine in the therapy of herpes simplex PubMed
- Herpes zoster infection prognosis Epocrates
- Ursini T et al, 2011, Acupuncture for the treatment of severe acute pain in Herpes Zoster: results of a nested, open-label, randomized trial in the VZV Pain Study PubMed Central
- Coyle ME et al, 2017, Acupuncture plus moxibustion for herpes zoster: A systematic review and meta-analysis of randomized controlled trials PubMed
- Cao H et al, 2010, Wet cupping therapy for treatment of herpes zoster: a systematic review of randomized controlled trials PubMed Central
- Semionov V et al, 2008, Post herpetic itching–a treatment dilemma PubMed
- Szabo G et al, 2009, A recent perspective on alcohol, immunity, and host defense PubMed


Got rid of Hsv,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,,
It worked for me,
Thank you!!!