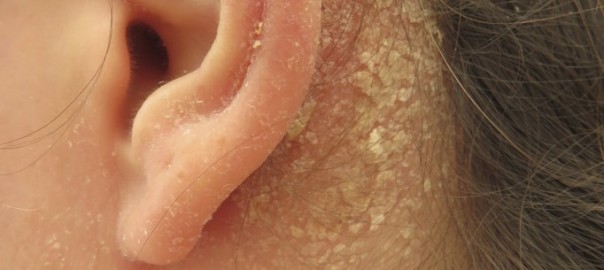
What is seborrheic dermatitis?
Seborrheic dermatitis is a common chronic inflammatory skin condition with greasy flakes and redness on the face, scalp or other parts of the body. Seborrheic dermatitis is not an allergy, is not contagious and is not harmful [3].
Dandruff is an uninflamed form of seborrheic dermatitis, which appears as small white flakes on the scalp [6].
Cradle cap is seborrheic dermatitis in infants.
Pityriasiform seborrhoeide is a severe form of seborrheic dermatitis that affects the entire body.
Synonyms: seborrhea, seborrheic eczema, seborrheic psoriasis [6]
Symptoms and Signs
Seborrheic dermatitis can cause one or more of the following symptoms [2,5]:
- Thick, oily, white, yellowish or grayish scales or plaques
- Skin redness
- Red bumps (superficial folliculitis due to inflammation of the hair follicles)
- Mild itch or burning feeling
- Widespread skin reddening and peeling called erythroderma (rare)
Symptoms can last for years and flare and clear without an obvious reason. Commonly affected areas are those with abundant oil glands: the scalp or scalp margin, forehead, eyebrows, eyelids (blepharitis), around the nose (in the nasolabial folds) and behind the ears, ear canal, mustache, beard, armpits, upper central chest, upper back, below the breasts, the belly button, groin, genitals and the area around the anus [2,5,11]. Seborrheic dermatitis does not affect the areas without sebaceous glands, such as the palms and soles [11].
Seborrheic Dermatitis On the Scalp
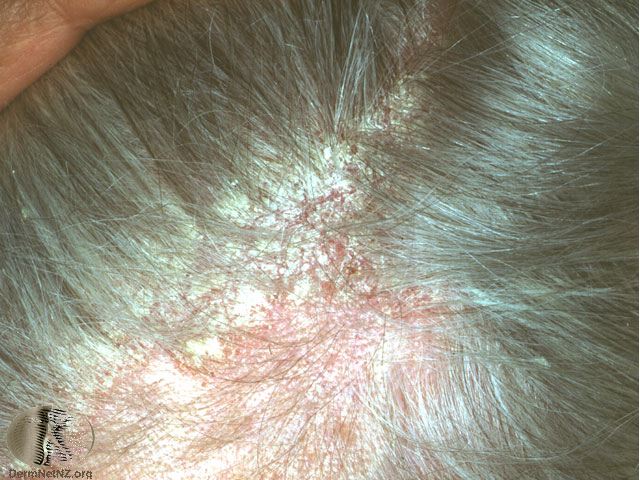
Picture 1. Seborrheic dermatitis on the scalp
(source: DermNet NZ, CC license)
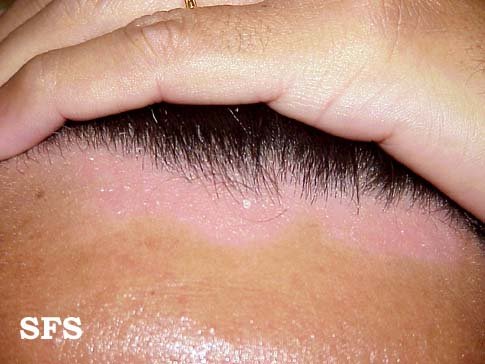
Picture 2. Seborrheic dermatitis along the hairline
(source: Dermatology Atlas)
Seborrheic Dermatitis On the Face
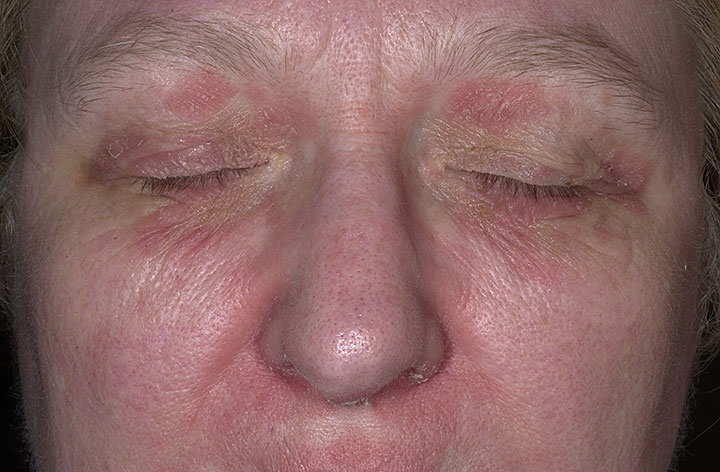
Picture 3. Seborrheic dermatitis on the face
(source: OMICS International, CC license)
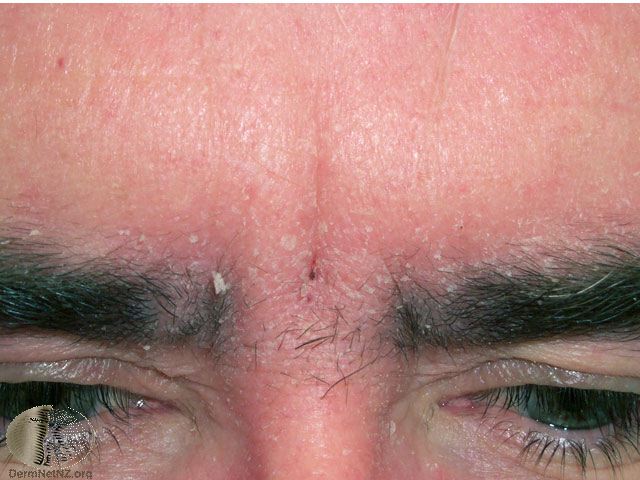
Picture 4. Seborrheic dermatitis in the eyebrows
(source: Dermatology Atlas)
Seborrheic Dermatitis On the Chest and Back
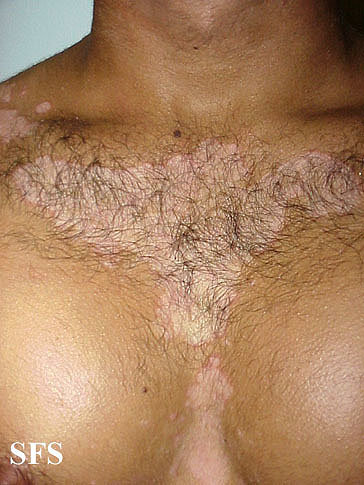
Picture 5. Seborrheic dermatitis on the chest (source: Dermatology Atlas)
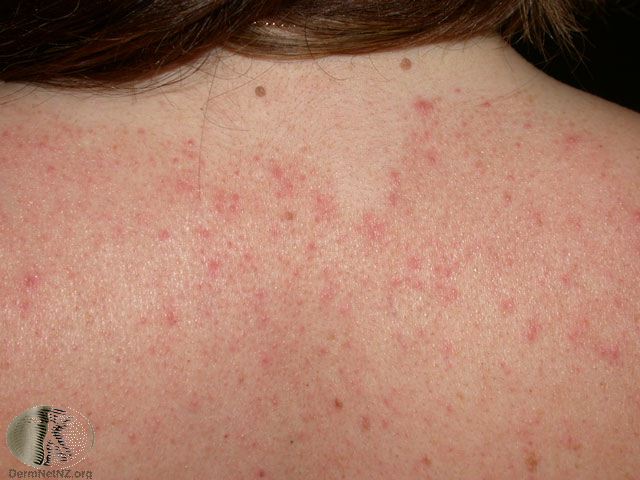
Picture 6. Seborrheic dermatitis on the upper back
(source: DermNet NZ, CC license)
Seborrheic Dermatitis Behind the Ear and In the Armpit
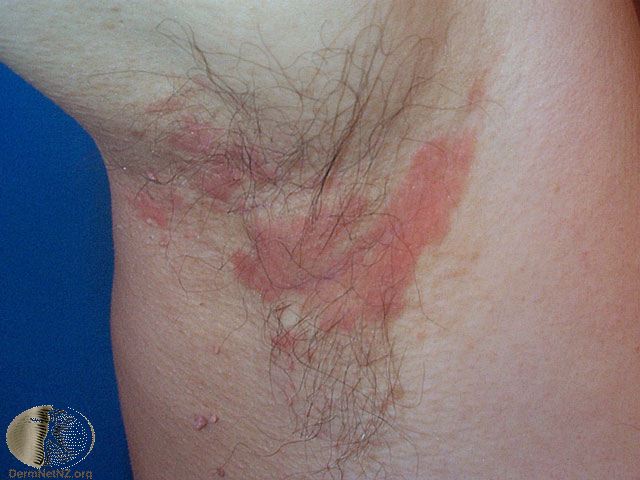
Picture 8. Seborrheic dermatitis in the armpit
(source: DermNet NZ, CC license)
Causes, Triggers and Risk Factors
Seborrheic dermatitis most commonly appears in infants younger than 3 months and in adults between 30 and 60 years of age [3].
The exact cause is not known; the risk factors can include [3,5,6,7,11,13,14]:
- Skin scratching and skin disorders, such as acne, rosacea and psoriasis
- Hereditary factors, such as sensitivity to otherwise normal skin Malassezia yeasts or its product oleic acid, which can result in a break of protective lipid skin barrier
- Hormonal factors (increased androgen stimulation of the sebaceous glands)
- Impaired immunity (HIV/AIDS, immunosuppression after organ transplantation)
- Neurological disorders (Parkinson’s disease, stroke, brain or spinal injury, facial nerve palsy, tardive dyskinesia, epilepsy)
- Deficiency of nutrients, such as vitamins B2 (riboflavin), B3 (niacin), B6 (pyridoxine), B7 (biotin) or zinc [9], commonly associated with alcoholism and eating disorders
- Other: obesity, fatigue, lack of sleep, depression, heart attack, congestive heart failure, alcoholic pancreatitis
Emotional stress, cold and dry weather and certain foods and medications (interferon, lithium and psoralen) can trigger a flare of seborrheic dermatitis [1,3].
Seborrheic dermatitis is not a sign of bad personal hygiene [1].
Differential Diagnosis
Conditions that may look similar to seborrheic dermatitis [7,9,11,18]:
- Allergic and irritant contact dermatitis
- Cutaneous candidiasis
- Psoriasis vulgaris (sharply demarcated silvery white scales on the scalp, nail pitting)
- Rosacea (redness, but no scales, on the cheeks and nose)
- Systemic lupus erythematosus or SLE (red “butterfly rash” without scales on the cheeks and forehead, swollen joints)
- Tinea infection or ringworm (alopecia: focal hair loss with broken hair)
- Erythrasma (red or brown patches in the armpits, groin or skin folds)
- Skin rash associated with a gastrointestinal disease, such as Crohn’s disease
- In children:
- Atopic dermatitis or eczema (very itchy scaly red rash on the scalp, forehead or face in infants)
- Impetigo (crusty red rash on the face due to a staph infection)
Treatment
The treatment, which includes anti-dandruff shampoos or antifungal and steroid ointments, can decrease the growth of the skin yeasts, remove scales and decrease itch. It is a dermatologist who can suggest which products to use and for how long. Treatment usually lasts for at least a month.
Outdoor activities with exposure to sun can decrease symptoms [5].
Treatment of Mild Seborrheic Dermatitis on the SCALP
There is MODERATE EVIDENCE that anti-dandruff shampoos, foams, lotions or sprays containing antifungals ketoconazole or ciplopirox [8,11,26,27] or steroids [11,27] can be effective in the treatment of the mild seborrheic dermatitis.
Treatment of Mild Seborrheic Dermatitis on the FACE
There is MODERATE EVIDENCE about the effectiveness of following in the treatment of the mild seborrheic dermatitis on the face:
- Antifungal creams or gels containing ketoconazole, ciplopirox or naftifin [8,9,11,19,21,23,26,27]
- Steroid creams containing hydrocortisone, betamethasone dipropionate, fluocinolone acetonide or desonide [11,19,23,26]. A common side effect with long-term (several weeks) use is thinning of the skin [19].
- Topical lithium gluconate or succinate [23,26]
- Immunomodulators pimecrolimus and tacrolimus (for persistent dermatitis; can cause hypopigmentation in black persons) [23,24,26,27]
Avoid products that contain alcohol, which irritates the skin. Petroleum jelly (soft paraffin) is not recommended [4].
Treatment of Moderate to Severe Seborrheic Dermatitis
Oral antifungals, such as itraconazole was effective in some studies [11,28,29].
Oral isotretinoin reduces inflammation and oil production by the sebaceous glands; it can be used when other therapy does not help [22].
Treatment Options with Insufficient Evidence of Effectiveness
There is insufficient evidence about the effectiveness of the following in the treatment of seborrheic dermatitis:
- Keratolytics and antifungals: azelaic acid [20], salicylic acid (with or without sulfur) pine tar, propylene glycol, urea, benzoyl-peroxide, zinc pyrithion or selenium sulfide [27]
- Moisturizers (emollients), including shea butter [25,27]
- Essential oils: aloe vera, arnica, jojoba, olive, peanut or mineral oil, tea tree oil [10,12]
- Supplements: vitamins B2, B3, B6 or C, fish oil
- Drugs: metronidazole (an oral antibiotic) [11,21], terbinafine (an antifungal) [25,27], fluocinonide (a steroid), antihistamines, antiandrogens (cyproterone acetate, spironolactone and flutamide [15,16])
- Phototherapy with UV-B light
- Dead sea salt
- Acupuncture
Prevention
- Avoid scratching.
- If you have a beard, shave it off.
- Do not use hair pomades.
- Wear loose smooth cloths to avoid irritation.
- Reference: 17, 19
Seborrheic Dermatitis in Infants
In infants, seborrheic dermatitis on the scalp is called cradle cap. The condition, which can also affect the diaper area or other parts of the skin, does not cause itch, is not dangerous and usually spontaneously disappear between the 6th and 12th month of life [1].
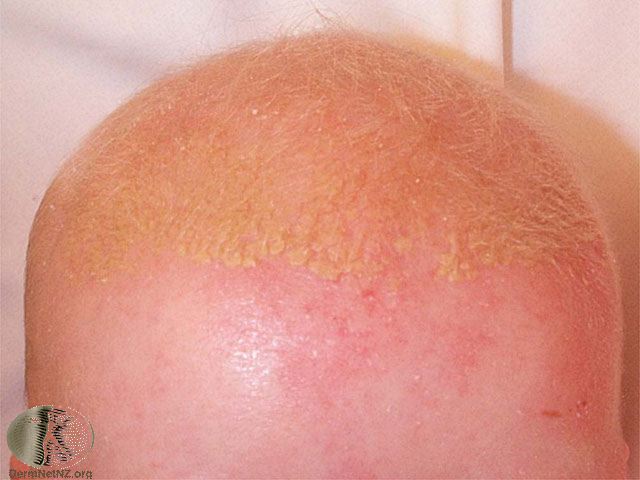
Picture 9. Seborrheic dermatitis (cradle cap) on the head of an infant (source: DermNet NZ, CC license)
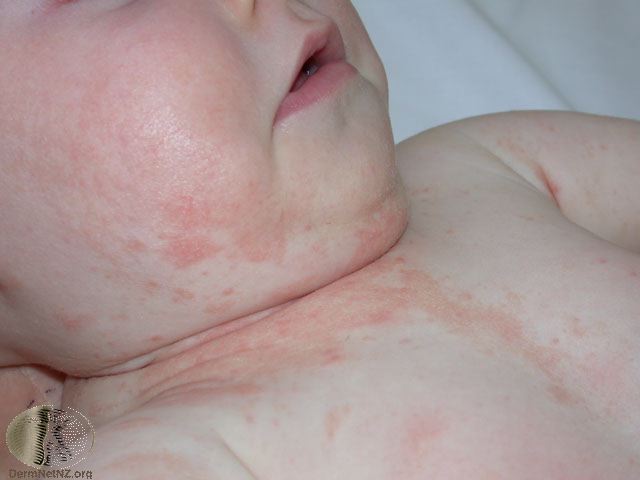
Picture 10. Severe seborrheic dermatitis in an infant (source: DermNet NZ, CC license)
Treatment includes baby shampoo and if this does not help, anti-dandruff shampoo. Before shampooing, you can apply warm mineral oil to soften the large thick scales.
Frequently Asked Questions?
1. How often should you wash hair with anti-dandruff shampoo?
If you have seborrheic dermatitis, you should wash hair according to instruction on the shampoo bottle or doctor’s recommendation. It is usually recommended to wash hair every day or every other day and for black persons once a week [4].
2. Does seborrheic dermatitis cause hair loss?
No [11]. Focal hair loss typically occurs in a fungal infection Tinea capitis (scalp ringworm).
- References
- Seborrheic dermatitis American Academy of Dermatology
- Seborrheic dermatitis, symptoms American Academy of Dermatology
- Seborrheic dermatitis, causes American Academy of Dermatology
- Seborrheic dermatitis, tips American Academy of Dermatology
- Johnson BA et al, 2000, Teatment of seborrheic dermatitis American Family Physician
- Seborrheic dermatitis DermNet NZ
- Seborrheic dermatitis: an overview American Family Physician
- Okokon EO et al, 2015, Topical antifungals for seborrhoeic dermatitis PubMed
- Sampio ALSB et al, 2011, Seborrheic dermatitis SciELO
- Satchell AC et al, 2002, Treatment of dandruff with 5% tea tree oil shampoo PubMed
- Borda LJ et al, 2015, Seborrheic Dermatitis and Dandruff: A Comprehensive Review PubMed Central
- Pazyar N et al, 2013, A review of applications of tea tree oil in dermatology PubMed
- Hoffman K, 2015, When Vitamin And Nutritional Deficiencies Cause Skin And Nail Changes Podiatry Today
- Seborrheic dermatitis risk factors Mayo Clinic
- Zouboulis CC et al, 2004, Androgen action on human skin — from basic research to clinical significance PubMed
- Singh SM et al, 2000, Androgen receptor antagonists (antiandrogens): structure-activity relationships PubMed
- Seborrheic dermatitis lifestyle and home remedies Mayo Clinic
- Handler MZ, Seborrheic dermatitis differential diagnosis Emedicine
- Handler MZ, Seborrheic dermatitis treatment Emedicine
- Bikowski J, 2009, Facial seborrheic dermatitis: a report on current status and therapeutic horizons PubMed
- Apasrawirote W et al, 2011, Topical antifungal agents for seborrheic dermatitis: systematic review and meta-analysis PubMed
- de Souza Leão Kamamoto C et al, 2017, Low-dose oral isotretinoin for moderate to severe seborrhea and seborrheic dermatitis: a randomized comparative trial PubMed
- 2015, Topical anti?inflammatory agents for seborrhoeic dermatitis of the face or scalp PubMed Health
- Ang-Tiu CU et al, 2012, Pimecrolimus 1% cream for the treatment of seborrheic dermatitis: a systematic review of randomized controlled trials PubMed
- Manríquez JJ et al, 2007, Seborrheic dermatitis PubMed Central
- Gupta AK et al, 2017, Topical Treatment of Facial Seborrheic Dermatitis: A Systematic Review PubMed
- Del Roso JQ, 2011, Adult seborrheic dermatitis PubMed Central
- Goldenberg G, 2013, Optimizing Treatment Approaches in Seborrheic Dermatitis PubMed Central
- Ghotsi SZ et al, 2015, Efficacy of Oral Itraconazole in the Treatment and Relapse Prevention of Moderate to Severe Seborrheic Dermatitis: A Randomized, Placebo-Controlled Trial PubMed
- Stefanaki I et al, 2010, Therapeutic Update on Seborrheic Dermatitis Skin Therapy Letter