What is a pilonidal cyst and where it is located?
A pilonidal cyst is a chronic benign (noncancerous) inflammation at the top of the crease of the buttocks, about 5 cm above the anus [1,2,9]. Although rare, a cyst can develop near the belly button or genitals, in an armpit or between the fingers [11].
The term pilonidal originates from “pilus” (hair) and “nidus” (nest) [7].
Pilonidal Cyst Symptoms and Signs
Pilonidal cysts are skin cysts that usually develop after puberty, most commonly between the age 15 and 25 [3].
In the beginning stage, a cyst appears as painless inflammation with one or more dimples in the midline of the tailbone area.
Later, a painful red lump (abscess) at the top of the cleft of the buttocks can appear. A pit located few cm below the lump can drain foul-smelling fluid, blood, pus or hair.
Tailbone pain is worse during sitting and is relieved by cyst draining, which can occur spontaneously [10].
Severely infected pilonidal cyst can come with fever or nausea [1,2].
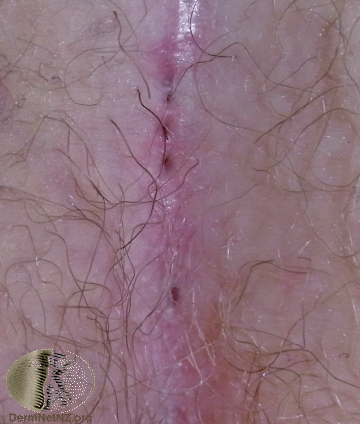
Picture 1. A pilonidal sinus with multiple dimples
(source: DermNet NZ)
Causes and Risk Factors
Pilonidal disease is considered an acquired disease with a possible genetic predisposition. Risk factors can include [1,2,3,10]:
- Being a white male between 15 and 30 years of age (pilonidal cysts can also appear in women and children, though)
- Repeated friction of the tailbone area from driving (in truck and military jeep drivers), cycling, office job or tight clothes, or an injury
- Poor hygiene and excessive sweating
- Previous infections (folliculitis, furuncle) on other parts of the skin
- Obesity, sedentary lifestyle
- Smoking [13,18]
- Deep crack between the buttocks
- Coarse, curly body hair
- Family history of pilonidal disease
Rarely, pilonidal cysts between the fingers develop in barbers, dog groomers and sheep shearers [11].
Mechanism
A pilonidal cyst usually develops from inflammation or infection of the hair follicles (bacterial folliculitis) or ingrown hair [1,3,10]. The infected hair follicles rupture and form an abscess under the skin. When the abscess heals, it leaves a cavity or canal (sinus) that opens to the skin surface with a small dimple [10]. An increased activity of the androgen hormones after puberty stimulates the development of pilonidal cysts [10].
A pilonidal cyst is not a true cyst because it is not completely lined with the epithelial cells, so the more corrects names for it are either pilonidal sinus or pilonidal disease [11].
A cyst can contain hair, parts of the skin and granulomatous tissue [3]. On the tissue and cell level (histologically), a pilonidal cyst is a foreign body type of hypersensitivity reaction [11].
Complications
When a pilonidal cyst becomes infected, it turns into an abscess, which appears as a red, tender and painful lump, which may or may not drain pus or blood. An abscess can burst spontaneously.
Rarely, a skin cancer (squamous cell carcinoma) can develop fro a pilonidal sinus [5].
Diagnosis
A doctor, usually a general practitioner or dermatologist, can make a diagnosis of pilonidal cyst by a physical examination.
Magnetic resonance imaging (MRI) can reveal the extent of a lesion and help to differentiate it from similar lesions, such as a perianal abscess.
Differential Diagnosis
Conditions that can look similar to a pilonidal cyst [4]:
- Boil (furuncle)
- Anal abscess with a fistula (common in Crohn’s disease)
- Hidradenitis suppurativa
- Congenital deformities of the spinal cord, such as spinal dysraphism
- Dermoid cyst or teratoma
- Pyoderma gangrenosum
- Tuberculous or syphilitic granuloma
- Osteomyelitis in the sacrum bone
Treatment
Painkillers
Over the counter analgesics, such as aspirin, paracetamol or ibuprofen, can relieve pain.
Home Remedies
Applying heat pads or sitting in warm water several times per day can provide some pain relief [12].
After a warm bath, you can gently massage the cyst and see if it will drain. Heat softens the greasy material in the cyst and thus allows easier draining. Remove any eventual liquid or hair that come out. Do not squeeze the cyst hard because it may rupture and later heal with an ugly scar. Do not poke or cut a cyst with any sharp object.
A coccyx cushion (doughnut cushion) or pillow can reduce pain during sitting [12].
There seems to be no reliable evidence about the effectiveness of Aloe vera, apple cider vinegar, baking soda, beeswax, black tea bags, Epsom salt, essential oils (tea tree, sage or castor oil), fenugreek, garlic, honey, neem leaves, turmeric, vitamin A or C, multivitamins zinc, in prevention or treatment of pilonidal cysts.
Surgery: Options, Recovery Time and Recurrence
It is usually a colorectal surgeon who removes pilonidal cysts. Most of the procedures described below can be performed in the outpatient setting.
An abscess (an infected cyst) can be treated in a doctor’s office by an incision, drainage and curettage under local anesthesia (Video 2). In most cases, the incision wound heals within 5 weeks, but an abscess can recur in as many as 50-85% cases because a doctor usually does not remove the cyst itself during this procedure [4,5,6,9].
A minimally invasive procedure called lay open, suitable for all types of pilonidal cysts, involves unroofing and curettage but no excision of a cyst [15,19]. According to one 2016 systematic review of studies, the healing time is 3-10 weeks, the average time for return to work 8 days and the recurrent rate 4.5% [16].
A pilonidal sinus can be removed by a complete excision, usually by a colorectal surgeon. The surgical wound can be closed by sutures; the wound healing time is 1-3 weeks and the recurrence rate can be up to 38% [8,9]. The wound that is left open without sutures can heal in 6 weeks to 6 months and needs changing the dressing few times a day [8,9]. The recurrence rate for an open wound is 10-20% [6,7,9,11]. One 2010 Cochrane review of studies has not revealed any clear benefit for open versus closed wound, though [14].
Marsupialization refers to forming a pouch by sewing the wound edges to the underneath muscle fascia and leaving the wound open [6]. Immediately after surgery, the wound looks like this. Healing lasts for about 6 weeks; the recurrence rate is up to 8% [9,11].
Bascom (cleft lift) procedure is described in detail here. It involves an incision laterally to the midline, excision of the pits and covering a wound with the skin flap from the other side of the crease that has been released from the underlying tissues [20]. The time for return to work is about 10 days [20]. The recurrence rate can be as low as 2.5% [21].
Other surgical techniques are described here and here. Most cysts are naturally cured until the age of 30 or 40 regardless of a surgical method used [9].
Home Care
A doctor should give you exact instructions about the after-surgery care, but in short:
- Maintain the area clean by having a daily shower or sitz bath.
- Keep the area dry and do not apply any ointments unless prescribed.
- Ask a wound care nurse how to dress the wound.
- Consume enough water and dietary fiber to prevent constipation and thus straining, which could result in the wound opening.
- Sleep face-down or on your side to prevent back pain.
Antibiotics by mouth or as ointments after surgery do not seem to reduce pilonidal cyst recurrence [9,11].
Doctors often recommend regular shaving of the tailbone area after surgery [1,22]. However, it is not clear if shaving helps to prevent cyst recurrence. In one 2009 study in 504 individuals, the recurrence rate among those who were using razors for epilation was 30%, and among those who were not epilating at all was 20% [23].
It is not yet clear if laser hair removal after surgery decreases the recurrence rate of pilonidal cysts [6,9,13,18].
Prevention
- Avoid jobs that involve prolonged sitting, such as driving.
- Avoid exercises that irritate the tailbone area, such as situps, running, cycling, horseback riding and backpacking.
- Lose weight, if you are overweight.
- Keep the tailbone area clean and dry.
- References: [1,6,13,18,22]
- References
- Pilonidal disease American Society of Colon and Rectal Surgeons
- Pilonidal sinus disease MedlinePlus
- Koyfman A, Pilonidal Cyst and Sinus, Overview Emedicine
- Koyfman A, Pilonidal Cyst and Sinus, Differential Diagnosis Emedicine
- Koyfman A, Pilonidal Cyst and Sinus, Follow Up Emedicine
- Rijoas RA, Pilonidal Cystectomy Emedicine
- Pilonidal disease DermNetNZ
- McCallum IJD et al, 2008, Healing by primary closure versus open healing after surgery for pilonidal sinus: systematic review and meta-analysis PubMed Central
- Spalding MC, Pilonidal Disease Treatment & Management Emedicine
- Spalding MC, Pilonidal Disease Clinical Presentation Emedicine
- Khanna A et al, 2011, Pilonidal disease PubMed Central
- Are there any home remedies for a pilonidal cyst? MedicineNet
- Ghnnam WM et al, 2011, Laser Hair Removal as Adjunct to Surgery for Pilonidal Sinus: Our Initial Experience
PubMed Central - Al-Khamis A et al, 2010, Healing by primary versus secondary intention after surgical treatment for pilonidal sinus PubMed
- Garg P et al, 2015, Laying open (deroofing) and curettage under local anesthesia for pilonidal disease: An outpatient procedure PubMed Central
- Garg P et al, 2016, Laying open (deroofing) and curettage of sinus as treatment of pilonidal disease: a systematic review and meta-analysis PubMed
- Yoldas T et al, 2013, Recurrent Pilonidal Sinus: Lay Open or Flap Closure, Does It Differ? PubMed Central
- Almajid FM et al, 2017, The risk of recurrence of Pilonidal disease after surgical management PubMed Central
- Kepenekci I et al, 2010, Unroofing and curettage for the treatment of acute and chronic pilonidal disease PubMed
- Stenberg J, Cleft lift procedure Pilonidal Surgery
- Gendy AS et al, 2011, A comparison of the cleft lift procedure vs wide excision and packing for the treatment of pilonidal disease in adolescents PubMed
- Uçar AD et l, 2016, Recurrent pilonidal disease surgery: Is it second primary or reoperative surgery? PubMed Central
- Petersens S et al 2009, Long-term effects of postoperative razor epilation in pilonidal sinus disease PubMed


Thank you for some other magnificent post. Where else may anyone get that
type of information in such a perfect approach of writing?
I’ve a presentation next week, and I’m at the search for such information.