What is a gallbladder polyp?
Gallbladder polyp is an abnormal growth that protrudes from the inner surface of the gallbladder into its lumen.
The polyps greater than 5 mm can be detected by ultrasound.
In about 5% of the cases, the polyps become cancerous [1].
Gallbladder polyps bigger than 10 mm are at increased risk to develop into cancer, so they are usually removed together with the gallbladder.
Types of Gallbladder Polyps
Gallbladder polyps can be benign or malign [1]:
- Benign polyps:
- Pseudotumors:
- Cholesterol polyps (most common, usually <10 mm, commonly multiple, with a stalk, do not develop into cancer)
- Inflammatory polyps (<10 mm, do not develop into cancer)
- Epithelial tumors: adenomas (5-20 mm, usually solitary and accompanied with gallstones, can develop into cancer)
- Adenomyomatosis – a benign noninflammatory lesion that can develop into cancer
- Mesenchymatous tumors: fibroma, lipoma, and hemangioma, leiomyoma, granular cell tumor
- Pseudotumors:
- Malign polyps:
- Adenocarcinoma
- Mucinous cystadenoma
- Squamous cell carcinoma
- Adenoacanthoma
Risk Factors For Polyps
- Age >60
- Female sex
- Gallstones
- Primary sclerosing cholangitis
- Chronic hepatitis B
- Congenital Peutz-Jeghers and Gardner syndrome
- Reference: [1]
Symptoms
In most cases, gallbladder polyps do not cause any symptoms, but sometimes they can cause:
- Pain in the right upper abdominal quadrant
- Nausea, vomiting
Polyps are often associated with gallstones [1].
Rare complications include acute acalculous cholecystitis, jaundice and cancer. Cholesterol polyps can detach, lodge in the common bile duct and cause pancreatitis [1].
Diagnosis
Gallbladder polyps greater than 5 mm can be detected by an abdominal ultrasound. An ultrasound can reveal the number and size of the polyps and distinguish between a cholesterol polyp and adenoma but cannot reliably distinguish between a benign and malign polyp (Picture 1) [1].
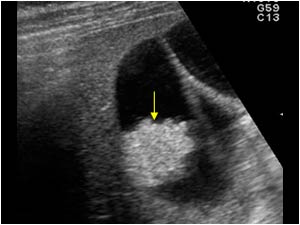
Picture 1. An ultrasound image (sonogram) of a 2 cm gallbladder polyp
(source: Ultrasoundcases, by permission)
Endoscopic ultrasound (EUS) (Picture 2) and high-resolution ultrasound (HRUS) seem to be equally effective in differentiating between benign and malign polyps [1].
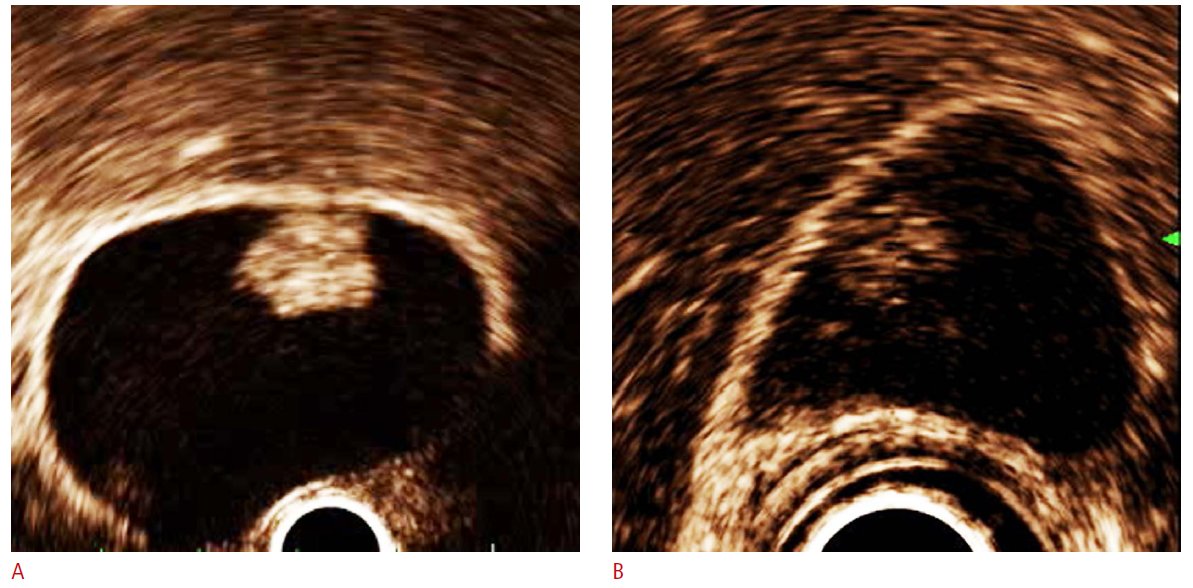
Picture 2. Contrast-enhanced endoscopic ultrasonography (EUS) of gallbladder adenoma – a benign tumor (A) and cholesterol polyp (B)
(source: Science Central)
Computed tomography (CT), magnetic resonance imaging (MRI) and intravenous cholecystography are less sensitive in detective gallbladder polyps than an ultrasound [1].
Risk Factors For Development Into Cancer
- Age >50
- Diabetes mellitus
- Gallstones or biliary sludge
- Primary sclerosing cholangitis
- Chronic infection with Salmonella typhi
- Porcelain gallbladder (calcification of the gallbladder wall)
- Polyp that is single, greater than 10 mm, without a stalk (“sessile”) and causes symptoms
- References: [1,2,5]
Treatment
A doctor will likely suggest gallbladder removal (cholecystectomy) when [1]:
- Cholesterol polyps and other polyps with low cancerous potential are greater than 10 mm
- Adenomas and other polyps greater than 6 mm are associated with increased risk factors for cancer
- Polyps of any size are associated with primary sclerosing cholangitis
A surgical technique of choice for the removal of the gallbladder with polyps is laparoscopic cholecystectomy [1]. In polyps larger than 18 mm, which are commonly cancerous, an open surgery with gallbladder, partial liver and regional lymph node removal is indicated [1].
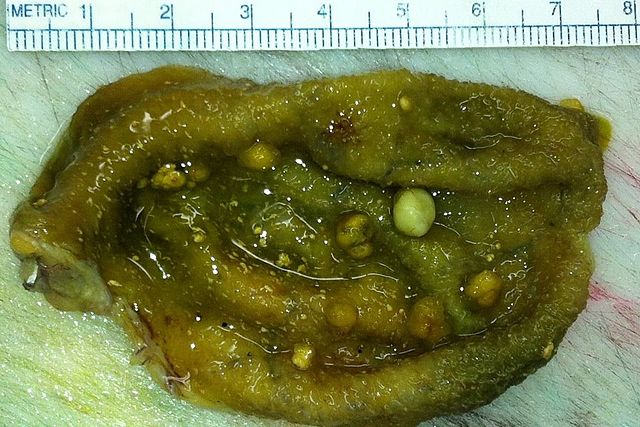
Picture 3. Multiple cholesterol gallbladder polyps in a removed and opened gallbladder (source: Wikimedia, CC license)
Follow-Up
Small polyps that are not removed should be followed up at regular intervals, for example, every 6 to 12 months [1].
Diet
There is no specific diet that would prevent gallbladder polyps. Since gallbladder polyps are commonly associated with gallstones, the diet that can help prevent gallstones may also reduce the risk of gallbladder polyps [3,4]. Main points:
- Maintain healthy body weight.
- Do not skip meals.
- If you intend to lose weight, do it slowly.
- Consume less saturated fats (red meat, cheese) and cholesterol (eggs, shrimps, organ meats).
Is it possible to flush gallbladder polyps?
There in NO EVIDENCE about the effectiveness of any drug, remedy or juice that would soften and flush gallbladder polyps.
- References
- Sandberg AA, 2012, Diagnosis and Management of Gallbladder Polyps PubMed Central
- VanderMeer TJ, Gallbladder tumors, overview Emedicine
- Gallstones prevention Mayo Clinic
- Dieting and gallstones National Institute of Diabetes and Digestive and Kidney Diseases
- Shaffer EA, Gallbladder cancer, the basics PubMed Central


i have gallblader polyps the size is 0.4 x 05 x 0.4cm what does it mean?
Sir my age is 21, I have a gall bladder polyp/adherent calculi with 5mm what can I do there is medicine for it ??last year it was 3r4mm is it dangerous can you give me a advice
Hello,
I am a 24 year old female. I have been experiencing severe nausea and right side of my head, headache pain. I have been for extensive testing and was found to have several small polyps in my gallbladder. My doctor was not concerned but i dont understand why he isnt. I have been so unwell for 3 months and have lost over 10 kilos. Surely the gallbladder polyps should be removed? Thanks in advance
Recently had an abdominal ultrasound…have been told that i may possibly have a polyp in gall bladder and have now been booked in for an MRI. Very worried….any advice appreciated.
I been expericing abdominal pain on my right side that shoots over to my left side. I been have it with some back pain and some trouble urinating. They did a ultersound and it came back that I had a 3mm polyp. Can this polyp be the cause of the pain and should I go through with removing the gallbladder like the doctor is suggesting that I do.
I also don’t feel like eating at times and have some nausea and gas. It is always tender right on the right side when I move or breath. I didn’t know if this could all be related to the polyp
i am 25… i have 4mm polyp in my gall bladder. Is any critical issue? what should i do for this? i don’t want to remove my gall bladder.. some doctors said there is no big issue.. its just normal.. i m vry worried about it when i heard about it will become cancerous ..
4 mm gallblader polyps are very unlikely cancerous. Currently, polyps are removed only by gallbladder removal.
i have this problm of 4mm polyps a year ago.. but still its size remain same.. tell me plss what should i do?
is there any point to worry? suggest me
The polyp remaining the same size after a year is a good sign. I can’t give a medical advice here. I suggest you to have another ultrasound after some time, according to a doctor’s advice. If the polyp remains about the same size it’s much lower risk for cancer. A polyp that is cancerous is usually bigger than 10 mm.
mam.. i have already scanned 5 times till now..
out of 5; 3 scan did not show any polyp in gall bladder. it showed ur gall bladder is normally distended with normal wall thickness.
should i do scan again??
The purpose of repeating scans is to check if a gallbladder polyp grows. In your case, it seems that the polyp did not grow bigger. POlyps smaller than 5 mm may be hard to detect by ultrasound, so this is probably why in 3 occasions, no polyp was detected. It surely makes sense to have another scan in the future but I can’t say when. You can ask the doctor who performed the last scan, what he/she recommends.
I was diagnosed with 9*10.4mm polyp…..Could it be cancerous…..other findings we’re normal….like no proclean GB..no wall thickening. Etc…..
It could be. Cancerous polyps are usually bigger, but even at this size they could be cancerous.
I was confined last dec, 23, 24, 25 of 2017 and diagnosed to have cholecystitis base from ct scan. I was confined to cure infection. But i was advised to have an early laparoscopic procedure. But its been 48 days had passed i never experienced any pain since i was brought to the hospital last dec 23, 2017. But after hospital discharged last Dec.25, 2017 and until now, I’m into a no fat diet food. I’ve finally made a followup check up for a 2nd opinion if i will be operated or not. The result of ultrasound was I have a gallbladder polyps of 0.8 cm. Im still not decided to do an operation. Is it possible that this polyps will grow or should be removed at once.
It is the next ultrasound after some time that can show if a polyp grows or not.
I have 5mm polyp in 2016, and just check back it become 9mm now in 2018. What should I do for this? Is this consider very fast ? I no suffer with any pain and not feeling any uncomfortable.
I don’t know, if it’s very fast, but it is obviously growing and it may continue to grow. Discuss with a doctor, about when to have next investigation and if you should have your gallbladder removed.
I have a polyp 10mm I see surgeon friday, this was only found 4 weeks ago! I have nausea loss of appetite and pain under right and left ribs .. I’m exhausted from constant pain.. I also have a few lumps along left ribs low down could these be lymph nodes ?
Lumps would be along the lower border of the rib cage? If so, they are not likely lymph nodes. The lumps may be from the intestine, for example from diverticles…
Hi. I have a 12mm polyp found in my gallbladder. I am nausea most of the time and get bad shoulder pain, don’t know if this is related? My dr suggest to wait 3 months for check up to see if it’s grown. Should I be worried? Do you know how quick it can grow?
When a polyp grows near the gallbladder’s neck, it may obstruct the cystic duct that leads out of it and cause symptoms similar to gallstones. This includes recurrent pain in the right upper abdomen, which can be referred to the right shoulder, and nausea that occurs only when pain occurs. Polyps can grow fast, I don’t know how fast, and it can be very different in each case. Polyps greater than 10 mm are suspicious for cancer. If the polyp grows further in 3 months, this means it grows fast. I personally would be worried, but you may discuss this with a doctor again.
I read my ultrasound report said, small polyp measuring 3 mm is seen posteriorly in the
gallbladder. Stones or biliary obstruction is not evident. Common bile
duct measures 3 mm.
My doctor called me said every thing is fine. I’m confused how is everything fine when they found something.
Gallbladder polyps as small as 3 mm usually do not cause any problems, especially if they do not grow with time. They are polyps greater than 10 mm that may develop into cancer. When you have a polyp, it is usually recommended to have another ultrasound after some time to check if it grows.
On 7th February I went for ultra sound,it was shown 2mm 2polyps in my gallbladder,again I went for ultra sound on 10th November..but the report says no calculus or any SOL is seen in lumen,is this possible or ultra sound machine problem
Sorry 4th November
It would be possible that polyps were not actually polyps but small stones. Such small stones may be spontaneously flushed out of gallbladder together with bile. On the other hand, 2 mm polyps may be hard to detect and easy to miss.
I have a 2mm gallbladder pylop. As mentioned in the above article, Consume less saturated fats (red meat, cheese) and cholesterol (eggs, shrimps, organ meats).
If I only eat egg white, will it make my pylop grow bigger?
Does protein cause pylops to grow bigger?
Thank you and looking forward to your advice.
The diet mentioned above in the article is for prevention of gallstones. I am not aware of any diet that would prevent the growth of a polyp when you already have it, especially if you do not have any gallstones.
I’ve been having pain where my galbladder is for years, in may I had an ultrasound and they said there was a small polyp in my galbladder, only one seen, (5mm) then I went for another one in September and the ultrasound tech said there was about 5 the biggest measuring 6mm , I have an appointment with a new gastro because I’ve been throwing up for the past 6 months, should I be concerned
Gallbladder polyps only rarely cause pain or vomiting, so I suggest you to ask a doctor if your symptoms could be from polyps, some other gallbladder issue or some other problem. Polyps 5-6 mm is size are rarely cancerous and rarely appear before age of 60.
Hello,
Im 30 i and i have been diagnosed with multiple polyps on gallbladder.
I have been refereed for gastroscopy. Doctor didnt explain why so i was wondering why?
I also don’t know why; you should ask the doctor before you go to the procedure.
Hi I am a 25 year old female. I recently had started to have somewhat severe pain that wouldn’t make me stop and take a moment till it passed. This happened for about a couple months before I decided to get things checked out. Turns out I have a 8.6 mm polyp in my gallbladder with no accompanying stones or other polyps. I’m assuming the polyp although most are asymptotic mine is causing me pain. How likely is it that it’s cancerous? I feel that with my age and the pain and larger size with no other polyps or stones that I may be looking st cancer.
An experienced gastroenterologist can better answer this. Most cancerous polyps are larger than 10 mm, but some smaller ones might be cancerous as well. Some polyps that are located near the gallbladder neck can block the bile flow out of it and thus cause temporary pain. Pain from cancerous polyp would be constant.
in ctmri
gallbladder appear distended and shows few hyper dense non-enhancing polyps attached to gallbladder wall largest polyps measure approx 6×6 mm along inferior wall of gallbladder
no definite evidence of adjacent gallbladder wall thickening or peri-gallbladder free fluid.
some slightly pain in Upperback side and abdomen.please give advice and allopathic or ayurvedic medicine.please reply
I’m not aware of any remedy that would cure gallbladder polyps. Gallbladder polyps of the size you mentioned are usually not dangerous.
sir any diet that can decrease size of polyps
There is no specific diet for gallbladder polyps, but you can read the recommendations above in the article.
Yesterday with ABDOMEN Ultrasound a non mobile echogenic focus without posterior acoustic shadowing measuring 2.1 mm in size was seen adherent to the posterior wall of my gallbladder, what does it mean, how should I proceed with the treatment of this. What could be the best treatment??? Should I further repeat some other lab test to further investigate……I am worried…please guide me in detail.
This sounds like a small gallbladder polyp, which usually, at this size, is not dangerous and is very unlikely cancerous. I’m not aware of any treatment for this. To remove such polyp, a doctor would need to remove the entire gallbladder.
Does apple juice can help curing gallblader polyps???
I don’t know about that. Gallbladder polyps are usually removed by gallbladder removal, when necessary.
I get ultrasound last week and the result said i have gallblader polyps..how can i cure this one
I had an altar sound done. I have a polyp just a little over a cm. 1.1. The doctor doesn’t seem to be concerned. I get a lot of pain in that area. Tenderness in stomach and feel nauseous at time. Don’t feel like eating at times. And can sleep at night. Should I be worried.
Sorry that was ment to say can’t sleep. Due to I worry about it. I can feel something there in my side all the time. I feel I’m emotionally tired and drain from it. I can’t get in to see a specialist til 3 months
I strongly recommend you to insist in having further investigations as soon as possible and NOT waiting for 3 months. Nausea, loss of appetite and tenderness in the gallbladder area are not normal.
i received ultra sound report for my gall bladder. they said the below thing:
” A 5 mm polyp versus sludge ball is seen within the gallbladder lumen. There is no evidence for calcified stone or cholecystitis.”
What should i understand what type of polyp is it?
To me, it sounds that the doctor thinks it is either a fleshy polyp or a clump of dense bile (sludge ball). A sludge ball may (or may not) develop into a gallstone.
Thanks Jan. Question: what do you mean my fleshy polyp? is it consider under adenomyometosis?
By a fleshy polyp I mean an overgrowth in the gallbladder wall that projects into the lumen…as opposed to a sludge ball, which develops from the bile and subsequently get attached to the wall and looks like a polyp. It is a pathologist who can say which exact type of the polyp it is – after gallbladder removal.
My close friend diagnosed with 5 mm polyp and does not have any gallstones. Is it true that if you have single polyp -it means is more chance to be having cancerous?
I wouldn’t know that…The risk of cancer increases with the polyp size. Polyps under 10 mm are not likely cancerous.
I had small gb polyp 4mm in the neck of gb but I don’t have any pain yet what should I do surgery is necessary or it dissolve by medicine.I consult with doctor he said to me keep medicine for 3 months and avoid fried food.what should I do now
What the doctor said sounds reasonable.
I had small Gb polyp 4mm, cause of that i feel sharp pain in my upper Abdomen ,back & on My side ,what should i do to reduce the pain and is surgery is necessary or it dissolve by any medicine.
Small polyps unlikely cause pain or any other problems. You may want to ask a doctor if you have gallstones. There are several non-gallbladder related causes of right upper abdominal pain, one of them is trapped gas, for example.
I had a growth of 4.7 mm polyp is it harmful
.
Polyps tend to grow and a doctor can say at which point the gallbladder needs to be removed. 4.7 mm by itself is not considered dangerous but a doctor can tell.