Where do you feel gas pain?
Gas usually causes pain in the upper abdomen and lower chest. The pain results from gas trapped in the part of the large intestine that runs below the rib cage.
What is trapped gas?
Trapped gas or trapped wind refers to a pocket of gas in the part of the colon that runs horizontally below the lowest ribs. Trapped gas can cause spasms in the colonic wall and the distension of the ligaments that hold the colon in the position, which can both cause severe upper abdominal pain.
Synonyms:
- Splenic flexure syndrome (the pain on the left side – near the spleen)
- Hepatic flexure syndrome (the pain on the right side – near the liver)
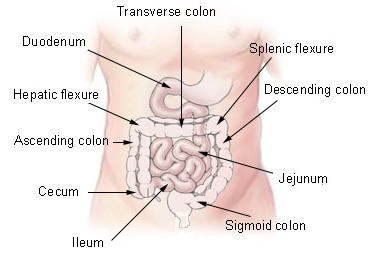
Picture 1. Splenic and hepatic flexure
(source: Wikipedia, CC license)
Causes and Triggers
The two main causes of gas pain are probably eating foods that irritate you and psychological stress.
Trapped gas often occurs in individuals with irritable bowel syndrome (IBS) and increased intestinal (visceral) sensitivity [1]. The pain can be triggered by:
- Big meal
- Constipation
- Emotional stress
- Air swallowing during drinking through a straw, fast eating or chewing gum
- Eating foods high in soluble fiber, such as legumes, oatmeal, barley, apples, pears or cabbage
- Drinking carbonated drinks or alcohol
- Pregnancy
- Drugs: antacids, antibiotics, antidepressants, antihistamines, opiates (morphine, codeine)
- Supplements: psyllium husk
- Colonoscopy
Serious underlying health disorders that can be associated with gas pains:
- Abdominal adhesions after abdominal surgery or infection or in endometriosis
- Diverticulosis or diverticulitis
- Ileus–temporary absence of the bowel motility, usually after surgery or in severe abdominal infection
- Bowel obstruction by a polyp, for example in Crohn’s disease or ulcerative colitis, or by colon cancer
Symptoms
Trapped wind can occur as a single event or as a recurrent or chronic problem. Symptoms may range from mild discomfort to debilitating pain and include:
- Constant pain (except at night) in the upper left or right abdomen or lower chest, on the side of the body or in the middle back lasting for several hours; it can be aggravated by sitting and deep breathing and eased by lying down, burping, passing gas or having a bowel movement [6]
- Distension (bloating) and tenderness in the upper left or right abdomen
Other symptoms, which may or may not appear along with abdominal pain, include referred pain in the tip of the left or right shoulder blade or down the inside of an arm, excessive belching, constipation, diarrhea, excessive gas (flatulence), nausea or dry heaving [6].
Trapped gas by itself does not cause fever.
Diagnosis
A doctor can often make a diagnosis of trapped gas by a physical examination. An X-ray image may or may not show an abnormal pocket of gas in the colon.
To exclude other abdominal conditions, abdominal ultrasound, colonoscopy or MRI may be needed.
Differential Diagnosis
If your main symptom is constipation:
- You may have a sedentary lifestyle
- You may drink too little water or consume too little insoluble dietary fiber (from whole grains and vegetables)
- You may be under stress
If your main symptoms are abdominal bloating and diarrhea, you may have:
- Fructose malabsorption
- Lactose intolerance
- Celiac disease
- Food poisoning
- Allergic reaction to food
- Infection of the stomach by the bacterium H. pylori
- Intestinal parasites
- Small intestinal bacterial overgrowth (SIBO)
- Diverticulitis
If your main symptoms are abdominal, chest or back pain and nausea, you may have:
- Acid reflux (gastroesophageal reflux disease or GERD)
- Gallbladder attack
- Biliary dyskinesia (either gallbladder dyskinesia or sphincter of Oddi dysfunction)
- Acute pancreatitis
- Acute appendicitis (pain near the belly button or in the lower right abdomen)
- Stomach or duodenal ulcer
- Gastroparesis (delayed stomach emptying)
- Kidney stones or other kidney disorder
- Disorders with enlarged spleen or liver
- Pleurisy
- Heart attack
- Low blood potassium level (hypokalemia) with painful cramps in the abdominal wall and calf muscles
- Shingles (Herpes zoster)
Treatment
NOTE: The information about the treatments presented below comes mainly from anecdotal reports and has not been evaluated by clinical studies.
Home Remedies
The following activities may relieve gas pain:
- Right after an onset of pain lie down, relax and massage the painful area with a hand.
- Pass gas or have a bowel movement.
- Deliberately change the speed of breathing.
- Drink warm water or hot peppermint or chamomile tea.
- Apply a heat pad for 10-20 minutes, several times a day.
Medications and Procedures
- Dicyclomine [3], hyoscyamine, propantheline and chlordiazepoxide/clidinium bromide [9] (antispasmodics) can relieve the spasms [3].
- Mild laxatives, such as magnesium citrate, or enemas, can resolve constipation.
- Digestive enzymes (lactase, lipase, amylase) can help in individuals with lack of digestive enzymes but not likely in others.
- Visceral manipulation (massage) performed by a physical therapist may result in prolonged pain relief.
- Colonoscopy can help release trapped gas.
Insufficient Evidence
There is no or insufficient evidence about the effectiveness of the following in relieving gas pain:
- Simethicone [2,5]
- Nonsteroidal anti-inflammatory drugs (NSAIDs): aspirin, diclofenac, ibuprofen, naproxen
- Paracetamol
- Bismuth salicylate
- Ginger [8]
- Activated charcoal [5,7]
- Stool softeners
- Apple cider vinegar
- Turmeric
- Gripe water (for infant colic pain)
Antacids (calcium carbonate), prokinetic drugs (domperidone, metoclopramide), prebiotics and raw food diet can aggravate gas pain.
Prevention
1. Be Active and Avoid Unnecessary Stress
Concentrate on work you believe is right for you and brings peace to your heart. In your desire to be successful with your work, you will feel the need to arrange your sleeping and eating habits and your relationships, which might greatly reduce stress and thus gas pain.
Physical activity often helps with bowel regularity. Walking can be fine; no need to go to the gym.
2. Diet
Try to avoid:
- Large amounts of foods high in soluble fiber, such as beans and peas, oats, barley, passion fruit, figs, bananas, broccoli, cabbage, cauliflower, onions, artichokes and sweet potatoes
- Artificial sweeteners sorbitol, mannitol, maltitol and xylitol found in sugar-free chewing gum and soft drinks
- Foods high in lactose, such as milk, yogurt and ice cream (if you have lactose intolerance) or foods high in fructose, such as honey, apples, pears and mangoes (if you have fructose malabsorption)
- Anything you believe may trigger pain: alcohol, caffeine, fried foods or other foods
If you are constipated:
- Eat more foods high in insoluble fiber, such as whole-grain bread and green vegetables (NOTE: in some individuals with IBS, insoluble fiber may aggravate symptoms).
- Avoid foods that may constipate you: soda, chocolate, desserts, cheese, ice cream, caffeine (coffee, tea, cola), white bread and other foods low in fiber [4].
- Drink enough water.
If you suffer from abdominal bloating and excessive gas, you may want to try a low-FODMAP diet.
Gluten-free diet helps to individuals with celiac disease but not likely to others.
3. Probiotics
During or after treatment with antibiotics, probiotics help maintain beneficial bacteria in your bowel (intestinal flora) and thus prevent bloating or constipation. Probiotics may not be helpful in other circumstances.
Key Points
- Gas pain probably occurs as a reaction to emotional stress and certain foods.
- Avoid unnecessary stress and foods, be physically active and adopt regular eating, working and sleeping pattern.
- It is easy to confuse gas pain, which comes from the intestine, with pain that comes from the gallbladder, so before considering gallbladder removal, ask for an abdominal ultrasound or other investigations to get the exact diagnosis.
- References
- Lehrer JK, Irritable bowel syndrome, clinical presentation Emedicine
- Simethicone Drugs.com
- Dicyclomine Drugs.com
- IBS triggers and how to avoid them WebMD
- Gas and gas pains, treatment and drugs Mayo Clinic
- Shafar J, 1965, The splenic flexure syndrome PubMed Central
- Suarez FL et al, 1999, Failure of activated charcoal to reduce the release of gases produced by the colonic flora PubMed
- Ginger WebMD
- Librax (with clidinium) WebMD


I have constant trapped wind down below, it feels like burning too. I have I B S and diverticulitis disease too. I love my food, which does not help. It’s so depressing, don’t know what to eat or take anymore. Help appreciated pleas. Carol
Good evening,I’m a 39 year old woman who suffers with a pain under my right ribcage for more than a week,I can’t breath,sneeze or than I get hurt,I can’t lay on my right than it hurts when I inhale it hurts,can you please tell me what can it be please
I have had excessive bloating & gas (even with extra probiotics) since a cycle òf antibiotics a few months ago. Recently I noticed, especially when lying down, what seems to be gas moving through my small & large intestines. If it is caused by gas, while moving through, it creates multiple lumps and recessed areas (like peaks & valleys) that I can watch move around, come up and then go down. Can be just 1 lump to 10 or 12 moving lumps/valley at once. If I push on them they either recess back or move elsewhere. So far I can’t find this symptom online, and I asked a Nurse Line, but she had no idea. Soooo odd, any feedback would be great! S.H.
I’ve had this pain in the top of my abdomen; some inches above my navel and it turned out to be trapped gas. It was soo painful! It comes and goes about every four months. I take a handful of baking soda and drink some water then I can feel the gas move in about 30 min.
Hello, I am a 17 year old female and recently I have gotten constant gas air trapped in stomach. This happened just around three weeks ago, before this I could eat dairy products and fruits just fine.
Just around three weeks ago, eating mostly anything I have makes me have excess air in stomach and I feel uncomfortable due to this. Even drinking water makes me have excess air and gas. I have tried to reduce my food and water intake but it does not seem to help much. I’m worried that this might get worse as time goes on. please help me find what it is
Definitly sounds like gastritis. I am on my second relapse of this right now. Mine is caused from chronic gerd. I would definitely see a Dr. Right away. Please don’t self treat…
I couldn’t even drink water either without gas build- up. Had too ripe a fibrous broccoli, not well-chews on my part I’m afraid with parts fermenting in my gut for over a month! Finally spoke to my doctor who prescribed Pepcid and my gas misery level went from 8/9 out of 10 to 2 that afternoon . I had bee consuming some to one via Roland’s hourly with minimal relief. She Instructed me to let my stomach heal and eat white and soft foods like bananas and mashed potato’s and veg broth, avocado, no cheese or red meat – 6 small meals to keep bloat from distending too much. After several days to add a good probiotic and prebiotic supplement but not to over do. Best for that to be done naturally with yogurt and sauerkraut and but not for a week or two- said to stay clear of veggies and acidic food and drinks and spices. Bland is key to allow healing. I’m optimistic. Hope this info helps someone. Good luck.
Hi I have just had surgery Monday just gone I had a eptopic pregnancy . But during theatre a mistake was made and they had to cut away 10 cm of my bowel . Since Monday I’m in agony because my belly is so bloated n to top it off I’m black n blue and really soar . Pls help me
Go to a doctor as soon as possible and do not ask for advice about this online.
I have pains low down on the left side and have to see a Consultant about perhaps having an endoscopy (up the way) soon. I don’t sleep well and my weight has dropped from 10 st 4lbs to 9st 6lbs since beginning of August. …I know I have IBS, and possibly pouches (Diverticulosis) as well. In fact, in the morning especially, I can actually feels lumps or swelling in that left side area.
….It is just a few inches to the left of the top of the hip or thigh bone. I would like to rule out this as being a kidney problem. Is kidney pain ever felt in the area of the downward colon, same as IBS area?
Kidney stones in the ureter could cause severe acute pain in the lower abdomen.
Kidney inflammation or some other chronic kidney disorder might also cause referred pain in the lower abdomen, but in this case the pain in the flank would be also likely present. Kidney diseases are often associated with cloudy or foamy urine.
Here’s the article about kidney pain.
I am a 46 year old woman I’ve had stomach problems for decades,18 abdominal surgeries now Dow almost three months I’ve been in severe pain constipation,I been in and out the E.R room so finally i been seeing a gastro doc.he has prescribed a handful of meds,nothing seems to really work now I’m having severe gas issues u can’t eat,sleep,barely drink,there’s no bower obstruction they did ct scans,xrays,ultrasounds bloodwork and nothing.i feel like I’m possessed I don’t know what’s happening to me .can someone help me figure this out? Thank you …
Did they make the test for small intestinal bacterial overgrowth? This can cause gas. try a low-FODMAP diet (search online).
Look up, acute intermittent porphyria. I had problems for years. It’s not detectable with regular blood tests and scans. Can be diagnosed with urine, stool, and DNA.
Yes, they are urine tests. You can check some online sources.
I have had the same issue for 25 years. It used to be sporadic and has now become a daily horrible painful experience.. no one can explain it. I’m currently seeing doctors at the university of Miami and so far everything looks normal but even water makes air get trapped in there. I hate eating.. I wish I could tell you something more. Sometimes knowing someone suffers as much as you makes you feel like you’re not alone. Good luck. Gripe water (for babies) works miracles when pepto and gas x and phazyme and Bentyl and protonics wont do the trick. Sometimes I’m a second shirt of impaling myself with a needle to expel the air myself. It’s torturous these days.
My names Tierra and im 23 years old I started having a ball rolling around back and forth from my chest and stomach I keep taking different gas relief medicine and i keep passing gas but it isn’t helping me. It started one day before my period that was exactly a week ago. It’s still here and it’s causing my chest to be sore. What should I do? Its also painful when it goes in my chest when I breath.
You can consider having a low-FODMAP diet for few days and see if it helps.
My sister had similar symptoms and her lung deflated. Long journey later…. they finally figured out she had endometriosis of the lung with her periods.
I have IBS-C since age 19.I am now 60.I have been abusing laxatives,mostly senna and cascara for many years.I now have such incredible gas retention,it is excruciating.I can pass fecal matter without releasing any gas.After 8 days the pain was radiating into my scapula area,groin,shoulder,cheat,neck and back.The main area of pain is my Splenic Flexure,which is the name of the exact syndrome I suffer.Two days ago my Dr. prescribed Librax for me to try. I took one dose before lunch. By 2:30,I actually felt the knot in my gut relax and the huge gas bubble start to move,and eventually allow me to pass some gas.The reason I know the pain is gas and the associated pain is because when I am able to expel, I have instant relief. Unfortunately this only happened once.Following day I took 3 doses with absolutely no result.I have tried every thing available,from Amitiza like drugs to anti-spasmodics,xanax and every variant. Untold homeopathic and herbal products.I have tried motility enhancing drugs like Reglan,even Ilopam choline(discontinued,old school)I’ve been laxative addicted for years and have never been like this before.This Spenic Flexure syndrome has totally ruined my life. I have not had a colonoscopy strictly because of the fear of having the huge amount of gas caused by the procedure stuck in my colon. Apparently even the Hospital emergency room cannot physically remove the gas,except by basically giving you a colonoscopy.I’m hoping there is something that I can do to give me at least a bit of comfort.
You may try to avoid foods high in soluble fiber (beans, barley, oats..) and try foods with insoluble fiber (whole-grain bread…).
I’ve had digestive problems for many years. Long story short- IBS-C. But nobody could offer any help like this page has. I wish I had seen this page years ago! Anyway, the low-FODMAP diet saved my sanity and my life. It’s not a cure, of course. But I can largely live my life as I want without the worst of the symptoms.
I don’t have any connection, financial or otherwise, with Monash University (creators of this diet) or anybody else. This diet worked for me like a miracle. Be careful, there is SOME misinformation about the diet online from unofficial sources. Plus their research and refinement of the diet is ongoing. They have a e-mail newsletter, an app for your phone, and a twitter: #fodmapchat. Also very educational. Really.
This information was so incredibly helpful!!!! I have had severe stomach problems for the past 2 months. I had a C-Scan and an endoscopy at the hospital – neither of them showed too much out of the ordinary. I literally look like I swallowed a basketball and the stomach pain is constant 24/7. My ortho. that I have been seeing for the past 20 years has set me up for an MRI. I hope to God it shows something..anything to explain the incredible stomach distention, enlarged liver, gastritis, severe pancreatitis, etc. Whatever is going on inside my abdominal area is NOT normal, for me or anybody. I just want the constant stomach pain to stop and to look and feel like my old self again.
Laura, you may want to try a low-FODMAP diet, which can help remove several causes of gas and bloating.
Hi guys in an awful way here. Stomach destention I really do look 5 months pregnant I’m a size 10 and everyone is congratulating me and asking when am I due. Can I ask how you get info on this low food map diet please is there a book or something.
It’s a lot of information about low-FODMAP diet online.