What is chalazion?
Chalazion (plural = chalazia) is an inflamed nodule in the eyelid that develops after an obstruction of a sebaceous gland [1].
Deep chalazion, which appears on the inner side of the eyelid, results from an inflammation of the meibomian glands–a type of sebaceous glands in the middle part (tarsus) of the eyelid.
Superficial chalazion, which appears on the outer lid surface, usually results from an inflammation of the Zeis glands–a type of sebaceous glands near the eyelashes [1].
A chalazion is not cancerous.
Word origin: from the Greek khalazion = small lump [4]
Pronunciation: “kuh-LAY-zee-on”
Synonyms: meibomian cyst, meibomian gland lipogranuloma, tarsal cyst
What does chalazion look like?
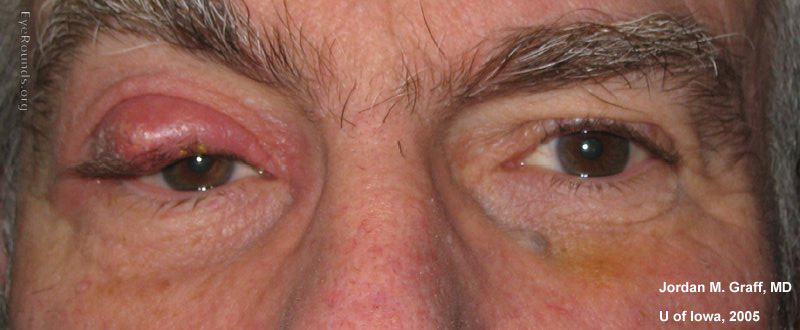
A chalazion appears as a small (2-8 mm), red, painless, nontender hard swelling in the eyelid [8]. It can be single or multiple and located in the upper or lower eyelid, on the outer or inner side. Fever is not typical for chalazion. An infected chalazion can be accompanied with a swollen lymph node in front of the ear. The inner surface of the eyelid is often reddened.
Picture 1. A large chalazion on the upper right eyelid
(source: Eye Rounds, CC license)
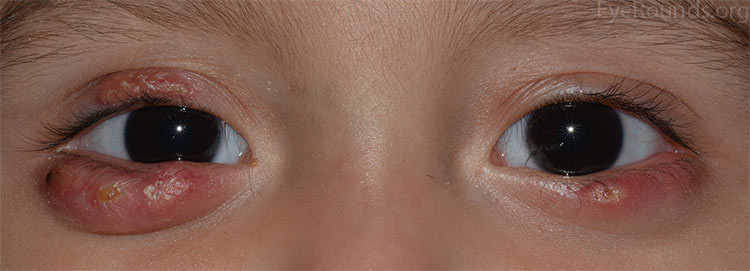
Picture 2. Multiple chalazia on both eyelids on both sides in a child
(source: Eye Rounds, CC license)
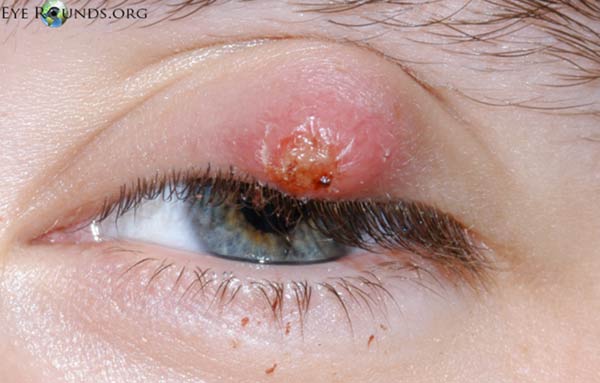
Picture 3. A chalazion on the upper left eyelid
(source: Eye Rounds, CC license)
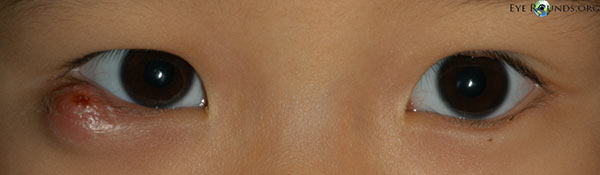
Picture 4. A big chalazion on the lower left eyelid in a small child
(source: Eye Rounds, CC license)
How long does chalazion last?
A chalazion often heals on its own within a month (2-8 weeks) [5,6]. If not, you can visit an eye doctor (ophthalmologist) to get an exact diagnosis and to exclude other conditions, such as cancer. An untreated chalazion can last as long as 2 years [1].
How does chalazion develop?
Bacteria, which normally live on the skin, enter the sebaceous glands and break down the fats in them. The breakdown products of the fat leak into the surrounding tissues and trigger an inflammation [1].
Chart 1. Chalazion Causes and Risk Factors |
|
|
|
Chart 1 sources: Emedicine [1,3], American Optometric Association [5], American Academy of Ophthalmology [7], GPnotebook [8]
What is the difference between chalazion and hordeolum (stye)?
A chalazion is a sterile inflammation while a hordeolum (stye) is an infection of the sebaceous glands.
Chart 2. Chalazion vs Hordeolum (Stye) |
||
| Chalazion | Hordeolum (Stye) | |
| Symptoms | Red, painless swelling | Painful red bump with white head on the lid margin |
| Duration | Chronic (weeks/months) | Acute (a week) |
| Common causes | Rosacea, seborrheic dermatitis | Staphylococcal infection |
| Pathology | Granulomatous inflammation | Infection (pus) |
Chart 2 source: Emedicine [1]
Complications
- Blurred vision because of irritation of the cornea or astigmatism – imperfect curvature of the eyeball
- Infection, including hordeolum (stye), pyogenic granuloma and cellulitis
- Eyelid depigmentation, disfiguration or eyelash loss
- Chalazion rupture, which can leave a scar
- Reference: [1]
Chart 3. Rashes and Bumps Similar to Chalazion |
|
|
|
Chart 3 source: Emedicine [1], University of Iowa [11]
Treatment
Home Remedies
Apply moist heat (warm compress) for 15 minutes 4-6 times a day for several days to soften the hardened fat in the sebaceous glands and to stimulate drainage [3,5]. Then gently massage the affected eyelid for few minutes. White greasy material coming from the inner side of the eyelid is a promising sign that a chalazion will heal on its own. This conservative treatment is effective in about 50% cases [3].
Do NOT try to pop or lance a chalazion on your own.
Drugs and Supplements
- Mild steroid drops
- For infected chalazia: oral antibiotics, such as doxycycline, minocycline or metronidazole for 10 days
- For individuals with chalazia and rosacea: oral antibiotics for 6 months
- For persistent chalazia: a steroid injection into a lesion can be effective in few weeks (possible complications: skin hypopigmentation or thinning)
- Antibiotic drops or creams are usually not used to treat non-infected chalazia.
- Reference: [3]
Chalazion Removal (Surgery)
It is an ophthalmologist or plastic surgeon who deals with the surgical treatment of chalazia. The procedure is outpatient and includes [3,11]:
- An injection of a local anesthetic into an eyelid (or general anesthesia in small children).
- Eyelid reversal using a clamp
- A vertical incision on the inner or, rarely, a horizontal incision on the outer side of the lid
- Curettage or excision of the inflammatory granuloma
- No sutures are usually needed since the wound heals without a scar.
- A doctor covers the eye with a gauze to collect eventual secretions and applies a topical antibiotic.
- Multiple chalazia can be excised during one appointment.
- A doctor can send the removed tissue for a pathological investigation to check for eventual sebaceous gland carcinoma.
Video 1. Surgical removal of a chalazion
Aftercare includes an initial cold compress for few hours, followed by warm compresses and antibiotic and steroid drops for a week. Do not massage the eyelid within the first month after surgery.
The effectiveness of the chalazia treatment [11]:
- A single steroid injection: 60-84%
- Second steroid injection: 77-89%
- A single incision: 79-87%
- Second incision: >90%
Complications during or after a surgical removal of a chalazion may include a rupture of the cornea, scar, fistula, an indent at the lid margin, an infection (orbital cellulitis), damage of the lacrimal gland.
Prevention
- After a shower, scrub the eyelids by hypochlorous acid, lavender, soap or baby shampoo, then vigorously massage the lids in a horizontal motion by “4 fingers times 10” routine: 10 rounds with the index, middle, ring and pinky finger [3].
- Use anti-dandruff shampoo or shampoo for seborrheic dermatitis on the eyebrows.
- Do not wear contact lenses until the chalazion heals.
There is INSUFFICIENT EVIDENCE about the effectiveness of the following nutrients and diets in the treatment of chalazia [3,9,10]:
- Essential fatty acids: omega-3 from flaxseed or fish oil (they may thin the oil in the sebaceous glands)
- Vitamin A in high doses, by mouth (it may work in vitamin A deficiency)
- N-acetylcysteine topical ointment
- Diet (avoiding chocolate, coffee, fried foods and foods high in saturated fats, such as red meat and cheese)
There seems to be no evidence about the effectiveness of applying apple cider vinegar, Epsom salt, Aloe vera, green tea bags in the chalazia treatment or prevention.
Recurrence
In predisposed individuals, chalazia tend to recur [2]. Recurrent chalazia should be investigated for cancer.
- References
- Deschênes J, Chalazion, overview Emedicine
- Deschênes J, Chalazion, presentation Emedicine
- Deschênes J, Chalazion, treatment & management Emedicine
- Chalazion Online Etymology Dictionary
- Chalazion American Optometric Association
- Chalazion and hordeolum (stye) Merck Manual
- Who is at risk for chalazia and styes? American Academy of Ophthalmology
- Chalazion GPnotebook
- Geerling G et al, 2011, The International Workshop on Meibomian Gland Dysfunction: Report of the Subcommittee on Management and Treatment of Meibomian Gland Dysfunction PubMed Central
- Gaby AR, 2008, Nutritional Therapies for Ocular Disorders: Part Three Alternative Medicine Review
- Kuiper J et al, 2014, Chalazion, Acute presentation and recurrence in a 4-year-old female University of Iowa Health Care