What is tailbone pain and where is it located?
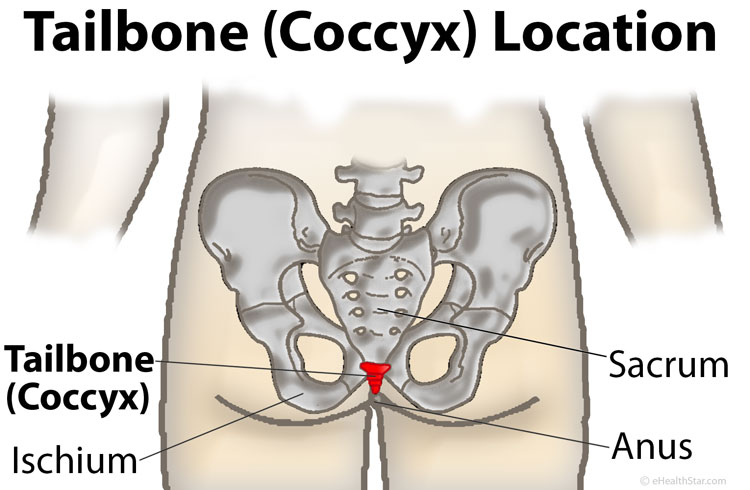
The tailbone or coccyx is the lowest part of the spinal column. It lies below the sacrum, beneath the buttocks crease. The bottom end (the tailbone tip) is about an inch (2.5 cm) above the anus and is bent slightly forward [1;73-p.329].
Picture 1. Coccyx location
Tailbone pain is any pain in the tailbone area. It can arise either from the coccyx bone or related ligaments, muscles, bursae (fluid-filled sacs that prevent friction), nerves or skin. When the pain arises from the actual coccyx bone, the coccyx will usually be sensitive to palpation; this is known as coccydynia, coccygodynia or coccyalgia (medical terms for tailbone pain) [7].
The pain is worst during sitting and when rising from sitting to standing position; some people describe it as sitting on a marble or knife [11]. The pain can be triggered by lying on the back, prolonged standing, walking, running, jumping, lifting heavy objects, sexual intercourse, bowel movement or even by coughing and sneezing, and can be relieved by leaning forward or to aside [13].
Common causes of acute tailbone pain are falls and childbirth and of chronic pain pregnancy and stress injuries (sitting, sport).
Risk Factors for Tailbone Pain
- Female sex [8,11]
- Sitting work: office work, driving [20]
- Sports with frequent falls on the tailbone (rugby, football, handball, wrestling, skiing, snowboarding, skating) and “sitting” sports (cycling, rowing, horse riding, care racing)
- Obesity [11]
- Rapid weight loss [15]
- Protruding coccyx–the tailbone sticks out as a hard bump above the anus [71]
Causes
Sudden (Acute) Pain
A. INJURY
Causes of tailbone injury include direct blow, fall, car accident and childbirth (especially when using forceps) [30,76]. A doctor can diagnose a tailbone injury by a physical examination. Investigations are usually not needed; to confirm a fracture, an X-ray is needed.
1. Prolonged Sitting
In some people, sitting on hard, but probably more commonly on soft, surfaces (office chair, sofa, car or motorbike seat), for as little as a couple of hours can cause a dull tailbone pain, which usually goes away as quickly as it has appeared; the pain may become chronic.
2. Contusion (Bruise)
- Symptoms and signs: dull pain that worsens with sitting, bruising in the tailbone area
- Treatment: cold compress or ice pack, analgesics, sitting on a U-shaped wedge cushion
- Recovery time: a skin bruise can disappear in 2-3 weeks, but pain can persist for several months, especially when a bone bruise develops.
- Reference: [70]
Without an X-ray or MRI, it is not possible to differ between a contusion and tailbone fracture.
3. Tailbone Sprain
Tailbone sprain means overstretching or rupture of the ligaments that connect the coccyx with the sacrum or pelvic bones [56].
- Symptoms and signs: tailbone pain aggravated by sitting, tenderness over the tailbone
- Treatment: injection of a steroid/anesthetic or sclerosant solution (prolotherapy) [56,76]
4. Tailbone Luxation and Subluxation
Tailbone luxation can be defined as the slipping (dislocation) of the coccyx vertebra by more than 25% after sitting, as determined by an X-ray [76]. In luxation, a coccyx vertebra is dislocated at both ends, while in subluxation, it is dislocated only on one end [76]. Symptoms are similar than in broken tailbone (see below).
5. Broken Tailbone (Fracture of the Coccyx)
- Symptoms and signs: cracking/popping sound, sudden, extreme, sharp pain, bruising and numbness in the tailbone area, inability to sit
- Diagnosis: X-ray
- Treatment: analgesics, sitting on a U-shaped wedge cushion; rarely surgical removal of the tailbone is needed
- Recovery time: pain may persist for 4-8 weeks or, according to anecdotal reports, as long as a year; in the beginning, you may also experience numbness during sitting
- Prevention: tailbone guards (protection pads), either separate or built into the underwear (padded shorts)
- References: [30,66,67]
Stress (hairline) fracture is a tiny crack in the bone; it is more common in female athletes and women with osteoporosis [75]. Hairline fractures may not be detected by an X-ray but only by a CT or MRI [75].
B. SUDDEN TAILBONE PAIN WITHOUT INJURY
Shingles–a reactivation of an infection of the spinal nerves by Herpes zoster virus. Symptoms: burning pain followed by a red itchy rash–that eventually crusts over–on the right or left side of the coccyx.
Anal abscess–a localized collection of pus due to an infection–, for example, in inflammatory bowel disease (Crohn’s disease, ulcerative colitis), rectal cancer or trauma, can cause throbbing pain in the coccyx area and, sometimes, swelling, redness, a lump with or without a visible opening (fistula) with discharge, and fever [64].
Medical procedures, such as colonoscopy, cystoscopy, spinal tap, epidural anesthesia, inserting of the intrauterine device (IUD), lower back surgery, curettage, hysterectomy or other pelvic surgery, can cause tailbone pain [21,61].
A coccyx infection (osteomyelitis) occurs very rarely; symptoms include severe dull pain, swelling and redness over the coccyx [31].
Persistent (Chronic) Pain
Chronic tailbone pain persists for more than 3 months [7]. A common mechanism is either tailbone hypermobility (flexion >25 degrees) [76] or hypomobility (flexion <5 degrees) [11,15] when sitting down, as confirmed by an X-ray.
1. Unexplained (Idiopathic) Pain
When a doctor can not find a cause of tailbone pain, the pain is called idiopathic [8]. Possible underlying conditions include increased front curvature (hooked coccyx) or side curvature (scoliosis) of the coccyx [19] increased [46,76] or decreased coccyx mobility due to the fusion of the sacrum and coccyx or fusion of the coccyx vertebra [15,47].
2. Coccydynia/Levator Ani Syndrome
- Causes: prolonged sitting in a soft chair, for example, in computer workers and drivers
- Symptoms and signs: tenderness and dull pain in the rectum, perineum (in the levator ani muscle), coccyx, vulva (vulvodynia), pubic area, buttocks and thighs that last for hours
- Prevention and treatment: initially, sitting on a ring or U-shaped wedge pillow and later, sitting on hard surfaces and having frequent breaks from sitting; it may take few weeks for the pain to decrease.
- Reference: [20]
3. Injury
Pain that persists for a prolonged time after an injury can be due to increased tailbone mobility or chronic inflammation and degeneration of the joints within the coccyx [7,8,11,16].
4. Myofascial Pain Due to Repetitive Stress
- Causes: cycling, driving, bike riding, horse riding, rowing, canoeing, sit-ups [27-p.125;45]
- Symptoms and signs: tight muscles in the lower back, muscle knots (trigger points) near the spine
- In gluteus maximus syndrome, a painful spasm appears in one buttock near the coccyx only when going from standing to sitting or from sitting to standing position or during squatting or sit-ups but not during sitting [49].
- Treatment: a massage technique called “myofascial release,” dry needling, injections of a local anesthetic into the muscle knots and spinal manipulation [56,73]
5. Other Causes of Chronic Tailbone Pain [7]:
Misaligned coccyx that points forwards and upwards (hooked coccyx) to the right or left (scoliosis) rarely causes coccyx pain [19,47].
Ankylosing spondylitis is an inflammation of the spinal vertebra (spinal arthritis) with the formation of extra bone and fusion of the vertebra. Symptoms usually start in early adulthood and include severe pain and stiffness in the lower back, tailbone and hips that decrease after moving around, and excessive forward bending of the upper spine (kyphosis) [43,44].
Calcium deposits in the tendons (calcific tendinitis) or the coccyx joints have no known cause; they can be successfully treated with corticosteroids (oral or injections) [23,24].
A pilonidal cyst is a chronic infection as a reaction to an ingrown hair. It can appear as a small pit, dimple or zit or a large, red, itchy, painful and tender soft lump or boil in a buttocks crease, 4-5 cm above the anus; it may be associated with a fistula that drains blood, pus or clear liquid [11,48].
Bursitis, an inflammation of the bursa–a fluid-filled sac at the tip of the coccyx–can cause chronic pain and tenderness in the coccyx; an injection of a local anesthetic can help [68,76].
Rare causes:
- Cancers in the tailbone, such as sacrococcygeal teratoma in newborns [51], sarcoma or chordoma [78], metastatic cancer from other organs, and rectal cancer
- Gout (uric acid arthritis) [14]
- Ehlers-Danlos syndrome (EDS)–a genetic disease of the connective tissue (stretchy skin, gastrointestinal problems and increased coccyx mobility with pain) [54]
Tailbone Pain in Pregnancy
During pregnancy, the ligaments and muscles in the pelvic floor relax due to increased secretion of the hormone relaxin [74], which results in increased tailbone mobility and thus pain [37,38]. In late pregnancy, a baby’s head pressing on the mother’s tailbone can further aggravate the pain. Pain can appear only in the third trimester or, according to some reports, as early as in the 15th week [17].
In symphysis pubis dysfunction, the gap between the pubic bones increases and can cause pain and discomfort in the pubic area, groin, inner thighs, sacrum or coccyx [38]. The pain can be aggravated by dressing, walking or climbing stairs. It can appear in the first trimester or only during labor and can persist for longer than 6 years [38]. Treatment may include physiotherapy, analgesics and epidural anesthesia [38].
Tailbone pain prevention in pregnancy:
- Try to sit on a donut or U-shaped wedge cushion. Padded underwear does not likely help because it increases the pressure on the tailbone.
- Kegel exercises are repeated contractions of the muscles around the urethra, vagina and anus in order to strengthen them and thus reduce coccyx mobility and pain [40].
- To learn how pelvic floor muscles work, try to hold urine during urination and stop the passage of the stool during a bowel movement. To do this, you need to contract muscles between the genitalia and anus. Technique [42]: At any time, when you are in bed, you are sitting or standing, but not during urinating or bowel movements, contract pelvic floor muscles as you were trying to hold the urine or stool. Hold for 5-10 seconds and release for 5-10 seconds. Do a set of 10 contractions and repeat several times a day.
- A physiotherapist can show you exercises to strengthen the pelvic floor muscles and thus reduce the coccyx mobility. Exercises may or may not reduce coccyx pain.
- A nonelastic maternity pelvic support belt can reduce pain in some, but not all, women [37,38].
- Allowed analgesics: acetaminophen. Drugs to avoid: nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or aspirin, steroids (both by mouth and injection).
- Severe tailbone pain during pregnancy may be a reason to consider a delivery by a C-section.
Referred Pain (No Tenderness in the Coccyx)
When you feel pain in the coccyx area but the pain does not worsen when you press on the coccyx, the pain probably originates from the nearby organs:
- Hemorrhoids. Symptoms: a bluish soft mass within the anus or protruding out, dull ache, feeling of fullness, burning and itching in the anus, occasional rectal bleeding.
- Benign tumors near the coccyx, such as glomus tumor, dermoid or epidermal cyst, schwannoma, lipoma, hemangioma or other tumors in the pelvis can cause a visible lump and chronic tailbone pain [25,32,33].
- Complex regional pain syndrome (CRPS) or reflex sympathetic dystrophy (RSD) due to overactivity or irritation of the ganglion impar (ganglion of Walther)–a small nerve nodule in the front of the sacrum/coccyx joint–can cause pain in the coccyx and sacral area, rectum and perineum [3,55].
- Tarlov cyst, which arises from the meningeal membrane that covers sacral spinal nerves, can cause soreness, burning sensation and feeling of pressure in the coccyx, sacrum, hip or thigh (sciatica), especially when bending forward [52,53]. It can develop after trauma or epidural injections; it can be diagnosed by an MRI [52].
Psychological Causes of Tailbone Pain
Tailbone pain is much more commonly caused by physical than psychological conditions [29]. Examples of psychogenic tailbone pain:
- Anorectal neuralgia–pain in the anus and rectum–may be associated with neurosis [22].
- Constant pain in the tailbone area that is not affected by the body position can be associated with hysteria or depression [76].
Other Causes of Pain Triggered By Sitting
Lumbar degenerative disc disease (spondylosis) with bulging or herniated discs L4/L5 or L5/S1 can result in a pinched sciatic nerve. Pain (sciatica), numbness, tingling and sometimes vibrating/buzzing feeling can radiate from the lower back toward a buttock, into the coccyx area, down the back side of the thigh and lower leg, into a foot and toes, usually only on one side. Symptoms are usually aggravated by sitting and relieved by walking [17].
In piriformis syndrome, the fall on the buttock can cause swelling and hardening of the piriformis muscle, which runs from the sacrum to the thigh bone (femur), and can press on the sciatic nerve. Pain, numbness and tingling can be felt in the buttock, coccyx, hip or groin, scrotum in men or labia in women. The pain can radiate down the back side of the leg (sciatica), usually only on one side, and can be aggravated by sitting, running, squatting or bowel movements [50].
Nonrelaxing pelvic floor dysfunction refers to increased tension of the muscles between the genitalia and coccyx (levator ani muscle). Causes may include forced holding of urine and stool for prolonged periods as learned from childhood, abnormal reaction to stress, postural or gait abnormalities, childbirth, injury, sexual abuse, pelvic surgery, irritable bowel syndrome, interstitial cystitis and endometriosis. Symptoms can include frequent urination or urinary urgency or hesitancy, constipation and painful intercourse [39]. Some people believe that squats are a good exercise to relax pelvic floor muscles. Squats strengthen the buttocks muscles, which pull the tailbone backward and thus possibly relieve pain.
Pudendal neuropathy (neuralgia) refers to a damage of the pudendal nerve in the pelvic floor, caused, for example, by an injury or diabetes mellitus. Symptoms may include stabbing or burning pain, tingling and numbness (paresthesia) around the genitalia, anus or the coccyx; symptoms are aggravated by sitting and relieved by sitting on a toilet seat or donut cushion [41,58].
Other Causes of Lower Back Pain
Immediate pain relief after injection of an anesthetic in the tailbone suggests that pain arises from the tailbone [11].
“Bad back” or “stiff back” can result from lower back injury; the pain is in the lumbar area, not likely in the coccyx.
In fibromyalgia, tender points can be found symmetrically on the right and left side above the buttocks, on the back side of the neck, at the top of the shoulders, in elbows, hips and knees but not over the coccyx.
Proctalgia fugax is random, sudden, sharp, stabbing, short-lasting (seconds, minutes) pain in the anus, usually at night, and is not related to bowel movements or bowel diseases [62].
Tailbone Pain Examination
Inspection and external palpation. A doctor inspects the area for eventual deformities or abnormal bumps and checks for tailbone tenderness.
Internal palpation. A doctor inserts one or two gloved fingers into the rectum, tests the tailbone mobility and checks for tumors.
Coccyx Pain Investigations
X-Ray
A dynamic X-ray in sitting and standing position can reveal an abnormal curvature or flexibility of the tailbone, fractures, subluxations, luxations or other dislocations and bone spurs (spicules).
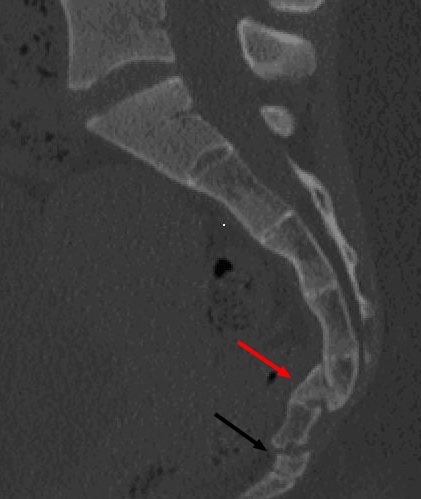
Picture 2. An X-ray of a coccyx fracture and subluxation
in a 34 years old woman after a fall from a bicycle
Red arrow: fracture
Black arrow: subluxation
(source: coccyx.org)
MRI
Magnetic resonance imaging (MRI) can reveal fractures, dislocations, tumors, degenerative spinal disc or joint disease, bone spurs or inflammation [11].
CT
Computer tomography (CT) is rarely needed; it can be used to better show suspected fractures.
Stool test for blood should be performed when rectal cancer is suspected [11].
Prevention, Treatment and Management of Tailbone Pain
Early treatment reduces the chance that acute pain will become chronic [6].
Appropriate Sitting Position
During the sitting, lean forward, so your tailbone will not bear the weight of your upper body. It can help if you alternately sit on the right and left cheek. Sitting always on one cheek can cause ischial bursitis–an inflammation of a fluid-filled sac on the bottom of the hip bone–and pain on the bottom of the right or left buttock [7].
After each hour of sitting, stand or walk for 5 minutes.
Seat Cushions
Ring (donut) or U-shaped wedge cushions prevent tailbone contact with the sitting surface and can thus prevent pain [15]. Many individuals prefer wedge over donut cushions, but some prefer neither [34]. Gel and inflatable cushions are available.
Special chairs that help prevent tailbone pain are available. If nothing other is available, you can sit on two chairs with one leg on each.
NOTE: Sitting on soft chairs usually aggravates, not relieves, coccyx pain.
Avoid Constipation
Try to avoid constipation by maintaining soft stools: consume enough dietary fiber (plant foods) and water [11]. Avoid straining during bowel movements.
Ice Packs, Heat Pads, Sitz-Baths
Ice cubs packed in a plastic bag and wrapped in a cloth, or heat pads placed on the painful area for 20 minutes several times a day may help reduce pain if you have bruised or broken tailbone [35]. Hot pads or hot sitz-baths may also help.
Stretching Exercises
If you have a fresh coccyx injury, do not do any exercises unless your doctor has told you so.
According to anecdotal reports, the following exercises may help reduce coccyx pain [40,77]: walking, squats, swimming on the back with minimal thigh movements, hands to feet stretch and kneeling groin stretch.
Oral Painkillers
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can reduce tailbone pain [6]. Analgesic creams applied on the skin over the coccyx may also be effective [15].
- Acetaminophen and tramadol can help.
- Pregabalin or gabapentin can be used in Herpes zoster infection (shingles) or diabetic neuropathy [6].
- Opiates fentanyl citrate or oxycodone can be used in severe pain [6].
Physiotherapy
Massage
Massage may help in muscle knots and nonrelaxing pelvic floor dysfunction [39].
Coccygeal Manipulation/Mobilization/Alignment
After an injection of a local anesthetic in the coccyx region, a doctor inserts a gloved index finger into the rectum and puts the thumb finger over the coccyx from outside and repeatedly flexes and extends the coccyx for about a minute [11]. Coccygeal manipulation can provide mild long-term relief, especially in combination with an injection of a local anesthetic, more likely in individuals with short-term pain and pain after trauma but less likely in individuals with immobile (fused) coccyx [5,12,17,26,56].
Kinesio Tape
According to one meta-analysis and one systematic review of studies (2012), there is insufficient evidence about the effect of kinesio tape (KT tape) in treating pain after muscle or bone injuries [69]. There seems to be a lack of studies about the effectiveness of KT tape in treating coccyx pain.
Acupuncture
There is a lack of studies about the effectiveness of acupuncture in the treatment of coccyx pain.
Injections
Corticosteroid (prednisone) injections–alone or in combination with a local anesthetic–near the joint between the sacrum and coccyx can be used to treat pain caused by an inflammation of the sacrococcygeal joint or ischial bursa [5].
Prolotherapy is used to strengthen sprained or partially torn ligaments after an injury. It involves an injection of the sclerosant solution near the affected joints [56]. The solution triggers proliferation (growth) of the ligament and thus strengthen it.
Ganglion impair blocks. A single injection of a local anesthetic lidocaine can, in certain chronic causes of tailbone pain (ganglion impair overactivity) provide immediate relief (within minutes), which can last several hours, and considerable long-term reduction of pain; repeated injections with longer-lasting anesthetics, such as bupivacaine, can provide relief lasting for months and significant long-term reduction of pain [5,55]. Injection of a botulinum toxin alone or in combination with a local anesthetic can provide longer pain relief that an anesthetic alone [59,60].
Destruction (ablation) of the ganglion impar. In persistent tailbone pain that does not respond to other treatment, destruction of the ganglion impar can provide long-term relief [5]. Individuals who get temporary relief from injections of local anesthetics will likely get relief from nerve ablation using phenol or ethanol injections or from radiofrequency ablation [5,55]. Sometimes, ablation needs to be repeated.
Sacral Nerve Root Stimulation
Spinal cord stimulation (sacral neuromodulation) by a small pacemaker-like device implanted under the skin in your hip area can relieve chronic coccyx pain, for example, after a coccyx fracture [57].
Surgery: Tailbone Removal (Coccygectomy)
Tailbone surgery can involve either the removal of only hypermobile parts of the coccyx or the entire coccyx. Surgery can permanently cure the pain in the following conditions [8,11,65]:
- Chronic tailbone pain not relieved by other treatment
- Cancer in the coccyx
- Unstable coccyx–luxation or subluxation–due to trauma or other causes [18]
- Coccyx that is permanently out of place
- Bone spurs
According to one source, in above conditions, surgery can relieve pain in up to 90% cases, but it may take 3 months to 1 year for a person to be pain-free [10,36].
In the following cases, tailbone pain will be less likely reduced by the tailbone removal [11,65]:
- No known cause of pain
- No tailbone tenderness
- No tailbone hypermobility (as determined by an X-ray)
- Pain in the lumbar area of the back
- Pain that radiates beyond the coccyx: into the buttocks or down the leg
Possible surgery complications [8,28]:
- Surgical wound infection
- Wound opening
- Intestinal hernia
- Pain persisting despite surgery
- Bowel incontinence
- Sagging of the pelvic floor muscles
Statistically, total coccyx removal is more effective and has fewer complications than partial removal [63].
- References
- Coccyx InnerBody
- Coccyx pain clinical presentation Emedicine
- Coccyx pain differential diagnosis Emedicine
- Coccyx pain workup Emedicine
- Coccyx pain treatment and management Emedicine
- Coccyx pain medication Emedicine
- Coccyx pain Emedicine
- Tailbone removal surgery Tailbone Doctor
- Coccygodynia Emedicine
- Coccygodynia treatment and management Emedicine
- Patel R et al, 2008, Coccydynia PubMed Central
- Maigne JY et al, 2001, Comparison of three manual coccydynia treatments: a pilot study PubMed
- Coccydynia Lahey Hospital & Medical Center
- Vossough A et al, A Unique Etiology of Intractable Coccygodynia Coccyx.org
- Smallwood Lirrete L et al, 2014, Coccydynia: An Overview of the Anatomy, Etiology, and Treatment of Coccyx Pain PubMed Central
- Balabin B et al, 2006, Coccygectomy for coccydynia: case series and review of literature PubMed
- Wray CC et al, 1991, Coccydynia The Bone and Joint Journal
- Pennekamp PH et al, 2005, Coccygectomy for coccygodynia: does pathogenesis matter? PubMed
- Kim NH et al, 1999, Clinical and radiological differences between traumatic and idiopathic coccygodynia Coccyx.org
- Marx FA ez al, 1996, Coccydynia/Levator Syndrome, A Therapeutic Test Coccyx.org
- Coccyx pain caused by previous medical procedures Coccyx.org
- Suduca P, 1985, Anorectal neuralgia PubMed
- Moon SG et al, 2012, Acute coccydynia related to precoccygeal calcific tendinitis PubMed
- Richette P et al, 2008, Coccydynia related to calcium crystal deposition PubMed
- Haasper C et al, 2007, Coccydynia due to a benign notochordal cell tumor PubMed
- Maigne JY et al, 2005, Treatment of chronic coccydynia (CC) by intrarectal manipulation. A randomized single-blinded study Coccyx.org
- Franzmayer C, 1999, Therapies successful on pain in coccygeal area Coccyx.org
- Zoon NL et al, 1997, Repair of a long-standing coccygeal hernia and open wound PubMed
- Foye P et al, 2010, Psychological versus Physical Pain Descriptors in Patients with Tailbone Pain Coccyx.org
- Maigne JY et al, 2012, Postpartum coccydynia: a case series study of 57 women PubMed
- Burnei G et al, 2007, Acute osteomyelitis–special cases with particularities related to specific locations PubMed
- Duncan L et al, 1991, Glomus tumor of the coccyx. A curable cause of coccygodynia PubMed
- Yang KC et al, 1989, Cystic sacrococcygeal lesions PubMed
- Foye PM et al, 2009, Coccyx cushions for tailbone pain: donut cushions versus wedge cushions Coccyx.org
- Treatment for coccydynia (tailbone pain) Spine-health
- Coccygectomy surgery for coccydynia (tailbone pain) Spine-health
- Francis M, What can I do to ease the pain in my tail bone? Parents.com
- Symphysis pubis dysfunction GPNotebook.co.uk
- Faubion SS et al, 2012, Recognition and Management of Nonrelaxing Pelvic Floor Dysfunction PubMed Central
- Exercise for coccyx pain Coccyx.org
- Prendergast SA et al, 2004, PT and PNE Jmweissmd.com
- Kegel exercises: a how-to guide for women Mayo Clinic
- Deniz R et al, 2014, Ankylosing spondylitis and a diagnostic dilemma: coccydynia PubMed
- Ankylosing spondylitis Spondylitis Association of America
- Travell JG et al, 1993, Myofascial Pain and Dysfunction: the Trigger Point Manual, Volume 2
- Maigne JY et al, 1994, Idiopathic coccygodynia. Lateral roentgenograms in the sitting position and coccygeal discography PubMed
- Idiopathic coccygodynia. Analysis of fifty-one operative cases and a radiographic study of the normal coccyx Coccyx.org
- Pilonidal cyst and sinus, clinical presentation Emedicine
- Muscle spasm or tightness causing coccyx pain Coccyx.org
- Piriformis syndrome Emedicine
- About sacrococcygeal teratoma The Children’s Hospital of Philadelphia
- Tarlov cyst information Tarlov Cyst Disease Foundation
- Tarlov cyst: case report and review of literature: Pubmed Central
- Ehlers-Danlos syndrome Coccyx.org
- Foye PM, Treatment of coccydynia by injection of local anesthetic to the ganglion Impar Coccyx.org
- Joint pain, coccyx The Pain Clinic
- Hope ER et al, 2012, Coccygeal Fracture Pain Cured by Sacral Neuromodulation: A Case Report Wiley Online Library
- Pudendal nerve and its pivotal role in pelvic floor dysfunction and pain International Continence Society
- Lim SJ et al, 2010, Ganglion Impar Block With Botulinum Toxin Type A for Chronic Perineal Pain -A Case Report PubMed Central
- Carrol I et al, 2009, Sympathetic Block with Botulinum Toxin to Treat Complex Regional Pain Syndrome PubMed Central
- Chiarioni G et al, 2011, Chronic proctalgia and chronic pelvic pain syndromes: New etiologic insights and treatment options PubMed Central
- Bharucha AE et al, 2008, Functional and Chronic Anorectal and Pelvic Pain Disorders PubMed Central
- Karadimas EJ et al, 2011, Surgical treatment of coccygodynia: an analytic review of the literature PubMed Central
- Anal Abscess/fistula American Society of Colon & Rectal Surgeons
- Maigne JY et al, 1999, Instability of the coccyx in coccydynia The Journal of Bone & Joint Surgery
- Fractured coccyx (tailbone) University of North Carolina Wilmington Abrons Student Health Center
- Tailbone trauma – aftercare MedlinePlus
- Maigne JY et al, 2011, Chronic coccydynia in adolescents. A series of 53 patients. PubMed
- Williams S et al, 2012, Kinesio taping in treatment and prevention of sports injuries: a meta-analysis of the evidence for its effectiveness PubMed
- Mostafavifar M et al, 2012, A systematic review of the effectiveness of kinesio taping for musculoskeletal injury PubMed
- Protruding coccyx bone Coccyx.org
- Dislocated tailbone Tailbone Doctor
- Giamberardino MA et al, 2011, Myofascial pain syndromes and their evaluation Best Practice & Research in Clinical Rheumatology
- Relaxin Encyclopaedia Britannica
- Stress Fractures of the Foot and Ankle OrthoInfo
- Maigne JY, 1998, Treatment strategies for coccydynia Coccyx.org
- Tail bone pain finally gone after 11 years Coccyx.org
- Understanding chordoma Chordoma Foundtaion


Hi, I am eleven years old, and I was at school and on the highest bars, I went to sit on it but as I was doing this I lost my balance and fell back onto my tail bone, hardly. I can hone from school after being in the nurses office for 3 hours. It just to sit, walk, couch, sneeze, and stand, so my school nurse said to get an X-ray but my mom said she things it’s fine, I’m trying to explain how excruciating the pain is but she says I’m fine. It hurts to bend down and I have to go to school tomorrow and these pages say to sit on soft surfaces but all day I will be sitting in a chair, hard, plastic chair. What do I do, what do I say to my mom to show her my pain?
About 15 years ago I had a fall down a flight of stairs. Couldn’t move for 2 days. At that time there was a huge clot in the coccyx area. After 2 days I was up and about with my usual lifestyle. About a week back I had severe pain starting from my bummies and radiating down my legs. Got an x-ray done… coccydynia. I’m right now on injections, medication and physiotherapy.
How long will the pain remain?
What do you advise me on my lifestyle?
I’m asked not to navigate the stairs… for how long?
Will the pain come back?
Do I need to wear a belt? If so what kind?
When can I travel?
Can I take flights?
I fell down some steps and fractured my tailbone (I got an xray to confirm). It’s healing well but there is a numbness around that area and I can’t feel the skin when I touch around that area either—is that normal/part of the healing process? Will this get better upon recovery?
i’ve recently been sick with a terrible cough causing a broken rib (thanks to child in day care). several days later, without injury, the area slightly to the left of my coccyx began to hurt, particularly on palpation or clenching glutes or contracting muscles in the groin area. this has continued for days. probably not pain like a fractured bone, but i have a high tolerance for pain and have mostly taken nothing for a broken rib
having moved slightly over a year ago to the pacific nw from ca, my activity and sunlight level has dropped big time. wondering if i have begun to get bone density loss? would that cause this?
further, is it possible to pull a muscle in the coccyx area by repeated coughing?
You can ask for investigations for bone density and osteoporosis. I’m not really sure if decreased sunlight exposure lasting for 1 year could cause significant decrease in bone density, though. But there may be some longer lasting underlying problem.
Coughing would not likely injure the coccyx or pull the muscle in the coccyx area, but coughing can trigger pain due to herniated discs in the sacral spine, for example.
Hi sir
I am parmar Ravi from Gujarat india I has been got pain in my secrume right side sience 6months
I took x ray pls give me ur mail id so I can send image
After seen x ray doctor told me
My tail bone touch to right hip
When I sit more than half an hour I m getting pain in my right but near to secrume
So pls guide me
I consult so many doctors but I didn’t get any solution pls help me
I can’t make a diagnosis from X-ray images here. What is your exact diagnosis – it must be written somewehere in the X-ray report or in other documentation.
I am a 25 year old normal weight active female. I was a hair stylist for five years until May 2017 I started getting severe pain in my lower back and tailbone. Both of my legs went weak and I was barely able to walk. When the doctors pressed on my lower back it was almost unbearable, however they stated that it didn’t feel broken so sent me on my way. I’ve had doctors tell me that it could be MS so I had a spinal MRI preformed as well as a brain scan. Both were normal however when reading my report it doesn’t state that the coccyx was visualized. Do they typically look at this area for an MRI? I have been trying to continue to workout and do yoga and physical therapy, however physical therapy has been triggering my leg weakness again. I went for months without pain but now it’s back I can’t sleep or sit comfortably. Muscle relaxers haven’t eased the pain, it is so awful it makes me feel nauseous when I stand up.
Please, do not do any exercises until you have such symptoms, especially if exercises worsen the symptoms.
Lower back pain in combination with bilateral leg weakness can occur in certain disorders of the lumbar spine or spinal cord. A herniated disc, spinal stenosis, arthritis or a tumor a few examples. From what you said, it is not clear where exactly was the tender spot – over the coccyx or higher in the sacral or lumbar area.
Coccyx bone conditions, including injuries, do not typically cause pain that would radiate down the legs.
Multiple sclerosis does not likely cause the pain in the lower back that would be aggravated by applying pressure.
One thing you can do is to collect your medical documentation and show it to someone who can explain what exactly was or wasn’t found by the investigations so far.
A few weeks ago I slipped in the shower (as dumb as it sounds its true) and I landed on a sharp tiled edge. I couldn’t walk for two days but pain persisted after weeks! What should I do?
A doctor can order an X-ray to see if coccyx is broken or damaged in some other way.
Need best hospital in india for spine tailbone pain.
Please tell how to get of bump near my tail bone between the butttucks.it is so pain full and I don’t sit comfortably and I can’t sleep well .It’s irritating me and I don’t what can I do know
The bump could be from pilonidal cyst, for example. Or from a coccyx bone injury. A doctor can help you.
Is it possible to bruise your coccyx by repeated heavy coughing over space of 5 -7 days?
No, that’s not likely. In someone who has a herniated disc in the sacral spine, cough could trigger pain, for example.
I injured my coccyx decades ago on parallel bars, falling from the bar directly onto my rear-end, almost blacked out. Now, on occasion, the pain will wake me up in the middle of the night, quite intense, to the point, last night, of almost blacking out and nausea. Seems to happen with weather changes, I broke out in a sweat but after 10 minutes it disapated. Took some ibuprofen, went back to bed, nothing this morning. Normal for this injury or not?
If the pain is in the middle, where the coccyx is, it could be related to the injury. It is an orthopedist who can judge about this on the basis of a physical examination and eventual imaging investigations.
i have been having issues for almost 10 months now. it started a just an annoying little pain in my butt. upper left butt to be exact. over time the pain ahs been worse and worse each time there is a flair up. i have had about 2 weeks of no pain, 3 times since oct. it feels like someone is putting a hot knife in the area of the spine just above the butt. there is a large hard knot to the left of that. my skin is so tender to touch. it doesnt hurt, in fact it almost feels good. if i apply pressure in the area surrounding it feels good. my tailbone sticks out far, and if touched it hurts bad. the rest of my spine is like that, also. it feels like compression in the lumbar to coccyx. i cant get comfortable, i cant sleep, its all i think about and it has consumed my life
Go to a doctor. Such pain can arise from the spine, ligaments, a cyst or tumor…
I have been suffering from coccyx pain for sometime now (around 3 months), I went to the doctor and he said that there is nothing up-normal in my X-ray. However I notice that I have the following:
1- Tenderness in the coccyx, at the upper edge of the buttocks.
2- Popping/clicking in the coccyx whenever I change postures during sitting this popping/clicking is accompanied with mild pain which disappears once the clicking is over.
3- when gently pressing the coccyx with my hand while sitting I can make it click.
The doctor suggested that I use donut pillow (which I have been using for a month prior to my appointment with him), apply heat pads, do exercises/aerobics and take a medicine called “Reparil” for one week.
Just to let you know, I don’t recall having an injury or trauma in the coccyx area, however my work requires me to set for prolonged periods which would be the main cause I suppose.
My question is, why would clicking and popping accompanied with mild pain happen and would the pain heal on its on by the measures mentioned above?
The pain I have is not major and doesn’t affect my activities much however what’s annoying is that I can’t sit with people on hard seats say when going out as I wouldn’t be comfortable sitting tilted forward all the time.
Such symptoms can be due to the coccyx hypermobility or dislocation, for example. An orthopedist who specifically deals with coccyx could tell more. In persistent pain, an MRI is usually recommended to check for exact cause.
I don’t want to interfer with your doctor’s treatment, but Reparil is used to “reduce swelling following injuries.” Also, if your symptoms are from repetitive strain due to sitting, there may not be exercises but rest that can help. Donut pillow seems reasonable, but if the issue persist, try to contact an orthopedist.
Thanks for the response, so in case I have hypermobility or dislocation, will these be healed overtime only by sitting on donut pillows and resting? when you suggested resting does that mean trying to lay on a couch or bed whenever possible? any other suggestions or measures that should be taken or that may help in healing?
Thanks again
By rest, I mean only avoiding heavy exercise and everything what can worsen the coccyx pain, for example, cycling, but not bed rest. You’ve mentioned that the pain started 3 months ago, so I assume you had some sort of injury or repeated strain…which possibly resulted in dislocation (because you mentioned clicking). Such dislocation may not heal on its own but I can’t say because I don’t know what really happened.
When you need to sit and can’t use a donut pillow, try to sit on hard rather on soft chairs. I’m not aware of any other helpful remedies or exercises. If the pain persists and you decide to visit a doctor, try to get an appointment with an orthopedist who specifically deals with coccyx.
By now, I am 100% healed, thanks to everyone who helped me with this, I received many advices some of which have really worked in my case.
Cheers
I think I banged my tailbone sitting on a mostly deflated airbed while camping.
That was 4 weeks ago. My tailbone is burning, I have to adjust my position often. Is this normal for bruising or should I still go to the doctor?
Tara
I don’t know. You may want to try to sit on *hard* surfaces or temporarily on doughnut cushions to allow the tailbone to heal. Use your intuition to decide to go to a doctor or not.
Hi,
I am a 30yr old female, BMI 21 with coccyx pain. At night I would state it was severe, during the day I am in constant pain but it feels more manageable as long as I don’t sit on it or walk up too many stairs.
Some background info: I work in the hospital and have been put on restricted duties due to issues with my shoulder and neck. My shoulder won’t rotate forward; a private osteopath thinks it is because my humerus is sitting too far forward in the socket. She also believes my neck pain is due to an irritated facet joint. I have a hospital appointment next month as my GP has referred me to the musculoskeletal team for investigation.
5 weeks after all this started my coccyx became painful. It is much more painful at night. I’m taking 30mg of codeine, ibruprofen and paracetamol 4-6 hrly and am still in a lot of pain, feeling unable to cope at night. It hurts sitting on it, lying on back, moving from standing to sitting (and back again), picking things up from them floor and walking up stairs. I am aware of it constantly but those activities definitely make it worse. The coccyx bone is tender to touch.
I have not had a fall and don’t sit for prolonged periods of time. I have been informed by GPs and physios in the past that I am hypermobile. I have also had a hip arthroscopy for FAI impingement and labral tear. The labrum was debrided and a portion of the ball of my hip was removed.
I am not sure if my issues with neck, shoulder, hip are related. Any ideas what I could have done/what my body is doing to me? Didn’t realise I’d be over the hill at 30!
Hypermobility is one of possible causes of coccyx pain. Other pains may be related or not. For pain at night you may try with different sleeping positions, cushings, etc.
The only Doctor I know that can treat Coccyx Pain is Dr Patrick Foye in Newark. go to his Website.
I had a local anaesthetic and steroid injection today to treat ciccydinia. The local anaesthetic was brilliant for a few hours I could sit down and sit back and stand after sitting without it hurting. Now a few hours later on my symptoms are feeling worse and have bowel movements and urinating more often. Is this normal after these injections and will the pain eventually get better? I have had coccydinia for about 10 months now and it brings me down slot with not being able to go to the cinema or sit properly at home or out in a cafe for examoke. Any advice would be very much appreciated. Thank you.
Local anesthetics provide only a temporary relief. The effect of a steroid injection can last longer but is also only temporary. I suggest you to find the exact cause of your pain with the help of your doctors.
Thanks for the quick response, I’m under my GP and they referred me to pain management team as MIR and x-ray shown nothing except inflammation and the continuous pain. Hopefully I will find out why I’m having these symptoms. Thanks again.
“Pain management team” might not be specialized enough…Some orthopedicians specialize in coccyx pain; you can search online…You can also think what happened 10 months ago: a fall, more sitting time, change of chair…Also, you can ask the doctor which are exact words that describe “inflammation.”
Thank you I will suggest this to my GP. 10 months ago I was working as a support worker and a lot of sitting on hard chairs for the training was unabarabe, I didn’t know it was coccydinia at the time I just assumed it was me and after the training sessions I was ok walking about. But 20 years ago I did have a hair line fractue in my lower spine and only a few years ago suffered pilosiditous, had that removed but no problems with that. Apart from them things I have nothing to say why or how I’m getting the pain in the coccyx. Doctor diagnosed me in December 2016 with coccydinia. It takes up all my life with everything I do. Just hope the steroid injection will work soon. Thanks again.
coccydynia, problem more than after .30 minitues sitting time in a chair, that problem is occure , pain in that area
One possible cause is a chair that is too soft.
Can mild scoliosis cause tailbone pain? I was diagnosed when I was in elementary school about 40 years ago. I was treated by a doctor in San Francisco until there were no changes. I have two curves one on the top back and one in the lower to mid-back. I am just curious. They are sending me to physical therapy. Thank you for your time!
I can’t say that scoliosis can not cause tailbone pain, but scoliosis, especially mild, does not typically cause pain in the upper back or in the tailbone. You may want to think of what other causes could be (sitting on a soft chair, etc…?)
I fell 3 years ago and I’m in pain since but now the pain is worst sit stand laying there’s always pain now it .moved to my pelves my bones is also paining all my jointsis getting difficult to do things in the house I’m trying to loose weight it might help I hope
Does anyone here experience pain in the front of the thighs..and groin area? Can a misaligned coccyx cause this pain ? Thank you….Im desperate…as many of you have been…and still are.
Such pain can occur in symphysis pubis dysfunction, usually during pregnancy, but possibly from other causes, too.
Where can you find a list of Doctors that specialize in Coccyx injuries, pain relief, or even surgical Dr.’s for removal of coccyx or consultation. I have not been able to find out this information. Please help me. Thank you.
Here’s one comprehensive list of doctors in various countries (and states within the US).
Hi, I started getting pain around my coccyx/sacrum about 5 weeks ago (no trauma). The pain is there nearly all the time but is a lot worse when sitting, getting up from sitting or certain positions. I went to the doctors and they said it was probably just the muscles around the coccyx/sacrum and gave me painkillers and muscle relaxants. It’s started to get worse in the last week and in the last couple of weeks I have started getting pins and needles in my hands and feet, as well as cramp like pains in my upper legs and buttock. I suffered an upper back injury 4 months ago but had no lower back issues with it. Do you have any suggestions to what it may be?
Danny, I strongly suggest you to discuss with your doctor about further investigations, for example, an MRI of the lower back. It is possible that something is pressing on the spinal nerves in that area and causing pain.
In many cases when pain is the only symptoms, the pain can arise from a damaged tailbone or from weak surrounding muscles. Pain associated with muscle cramps and pins and needles can suggest a neurological origin of pain.
My wife Mary fell on the sidewalk as a teen ager and landed on her tailbone back in 1958. When our son Mark was born in 1968, she broke her tailbone during his natural birth delivery . She had a bladder biopsy in 2000 and woke up with pains in her tailbone and sacrum. That pain has never let up since and it constantly plagues her to this day. She can’t stand, sit or lay for any length of time but must keep moving constantly so she can get some relief from the pain. She can not ride shotgun in a moving vehicle but must lay in the back on an air mattress to go from place to place. She also has fibromyalgia and has had it since 1996. i have searched the internet for years to see if anyone has had a similar experience with the sacrum & tailbone pain with fibromyalgia. If anyone has any suggestions as to how she can overcome these pains, it would be most welcome. She has gone to every kind of medical practitioner you can imagine but no one has any answers to alleviate her pain and suffering.
I’m not sure if I can make any comment.
Hi there I’m Rikesh I had spinal fusion on my L5 S1 but I suffer from coccyx pain terribly I had done an MRI and doctor says it’s clear and I’m making this up because I don’t want to work how dumb is the doctor if he don’t know his job horrible neurosurgeon
You can show the MRI image to another doctor and ask for a second opinion.
This is an excellent article. A few comments:
*Most sufferers feel aggravated by donut cushions and most find special coccyx cushions that are not those simple wedges far better but it is trial and error. Don’t get a donut cushion.
*The psychological causes are pure theory ie you can’t prove hysteria or neurosis causes coccyx pain and the article should delete that section as many sufferers get told such things only to later have a scan ie a dynamic sit/stand XRay or special coned down CT that shows the problem if they are lucky enough to find a good specialist. See coccyx.org for a list of doctors and PTs etc.
* Physiotherapy exercises to tighten the surrounding muscles can help in some cases but in others can aggravate if the muscles are too tight internally in response to an injury.
*The reference to 90% surgery recovery is one view and it is not 100% reduction and could be as low as 5% whilst some people end up much worse. It is classed as high risk surgery
Bernadette, how do you know all this? Are you an orthopedist, physiotherapist or you have researched this? I know coccyx.org. Do you have any other sources?
Hi again,
Thank you for the prompt answer yesterday.
Regarding that question from yesteday, I would like to know, by pressing with fingers on my bottom side while on a cat pose, could I hurt myself somehow and make dislocation or a nerve damage on the coccyx?
Also, is there any exercise to support the muscles and put the tailbone on the correct position itself and speed the self healing process?
Thank you
If you pressed hard on the coccyx, this could move a part of coccyx an cause pain. Before a doctor tells you an exact diagnosis (after an MRI), I would not recommend any exercises because you can make things worse.
Hi,
I fell down the stairs on 20th dec,after ibuprofen,ice and on 22nd Dec long flight to Cuba (almost a day),in a few days I was back to normal, dancing, walking and no painkillers. On 1st Jan I hit my tailbone very strong on the edge of a plastic sunbed. The pain came in a few hours, annoying but no severe. I took some neurofene,ibuprofen and did not stop walking and on 6th came back with a neck pillow under , and the pain got worse.suddenly in 2 weeks time from 15th Jan the pain disappeared and I felt much better, I started proper walking, even stretching exercises. In a week time, on 22 Jan, I decided to do an investigation of my bottom palpating with fingers(not very gentle) and happily realised that no pain or sensitiveness has been left,until I press in a place(where I think I hit myself the 2nd time) and a pain came strait away. Since than I am in a constant pain,presure and pinching burning pain around anus ,on the bottom like I have muscle strain and wright joint painful,Ibuprofen 400mg doesn’t work,,Started Naproxen,same. Xray has been refused,because it is a lot radiation and images not very clear,Waiting for lumbar and sacral mri.
What do you think that could be done, bruised or fracture and what do I need to do to prevent a chronic pain?
Irena, you may want to wait to the MRI results, which can show is it bone bruise, coccyx dislocation, fracture or something else. In meantime, you can try some doughnut pillows and avoid prolonged sitting.
I fell at work as I was dragging a recycling bag and tripped over a paper shredder I felt three pops when I fell. I went to the the doctor and he adjusted the tailbone, it felt great for ten days and then I went horseback riding no one said not too so dumb. The next day my world changed. I had the tail bone adjusted again by my doctor and later by my chiropractor
The pain is unbearable most of the time. If I do not exercise it is better. My pain is more in the vaginal area almost feels like a stick up there it is so awful I am almost thinking that I could have a cyst. I had a MIR but they did not get the whole tailbone however my lower lumbar is fine.
The next step is a c scan of the tailbone. Any thoughts??
Carla, it is certainly important that you get an exact diagnosis: is the tailbone broken or dislocated, for example, so more having a more detailed image of the coccyx seems reasonable.
Hi everyone, just in case this article did not go over how you can help it your tailbone feel better. What I did was put a heating pad where it hurts and stayed in a straight position spine too with a pillow and relaxed for a couple hours I would sugest 3 to 4 hours or sit up straight in a chair, I would still recommend going to the doctors due to a EXTREMELY RARE case of CANCER or BONE DAMAGE my tailbone was simply just bruised and needed healing if you go to the doctors they would sugest a MRI or XRAY scan to make sure it’s not broken or have cancer. Getting back to how you can make your tailbone feel better is staying in bed for a couple of hours with a heating pad. Make sure you are straight legs together. My pain was caused for sitting incorrectly at my desk. Slouching would do that aswell, while the pain can give you headaches and such you can take Tylenol or acetaminophen but please continue to stay in bed while you take it.
I have a tailbone pain exactly on the tip of the bone and slightly on the left side of the bone when I get to press on it hard. Light pressure with my finger doesnot make feel painful. Prolonged sitting gives me a knife-like pain while prolonged standing makes suddenly feel fatigue and a bit dizzy. Walking or moving around doesnot pain me. Also I had my right knee popping with sound and a slight pain whenever I bend it. No trauma I can remember. Had done x-Rays laying on my back and laying on my side with bending knees which showed nothing out of normal. The pain aggravates some days even I can feel something nagging when I lay down but still I can sleep, and other days the pain is very mild but it is there. A way back before many years I had my thyroid gland checked and it wasnot functioning correctly. I did it because I used to suffer from constipation. Now I don’t, but might it be a reason?!! Also I have taken a couple of years back vitamin D injection so I guess I don’t lack that. What should I do?!!
Aliaa, for a coccyx pan, you may want to find an orthopedists who has some experience with treating the coccyx. An orthopedist can tell you an exact diagnosis and what to do next.
I had twice fall more than 15 years ago ,I have been diagnosed with old fracture or hairline by MRI. It is such a really bad pain ,is killing me ,not be able to sit even for less than hour ,I am suffering a lot ,it also affect my life with my hosbanb as always complain ,I have got it most of the time ,just some time I have relif.I have fibromyalgia and family stoprosis history and adrenal fatigue as well (hole pakage ??). It’s getting worse in winter ,any way how can I know the fibromyalgia can cause my pain or the fracture can couse my pain ,and also what can I do as treatment as I can not stand any more by the pain . I am 45 years
Thanks
I had twice fall more than 15 years ago ,I have been diagnosed with old fracture or hairline by MRI. It is such a really bad pain ,is killing me ,not be able to sit even for less than hour ,I am suffering a lot ,it also affect my life with my hosbanb as always complain ,I have got it most of the time ,just some time I have relif.I have fibromyalgia and family stoprosis history and adrenal fatigue as well (hole pakage ??). It’s getting worse in winter ,any way how can I know the fibromyalgia can cause my pain or the fracture can couse my pain ,and also what can I do as treatment as I can not stand any more by the pain . I am 45 years
Thanks
Haleh, a knowledgable doctor, coccyx surgeon if possible, should be able to tell if your pain arises from the coccyx, fibromyalgia or something else. This means, first you need to get an exact diagnosis. Then a doctor can suggest the treatment.
I had a fall at wrk on a slipper tile floor n I went straight on my bum it’s 4weeks now still very painfull drive ,sit or stand doing phisio bt stil doesn’t help.plz help me
Subhnam, a doctor can tell if it only a bruise or did you break the coccyx bone. I don’t think any exercise will help. You may get a doughnut cushion to help you sit.
Injured tailbone initially after childbirth 32 years ago. Reinjured it after jet skiing 10 years ago. I have had cortisone injections on and off since. Last time the shot did not work and the skin is compromised in that area now. Did PT but did not help. Spine surgeon did not recommend coccyx removal beccause of the nerves and the skin issue. I am looking into a tens type machine to be implanted but did not get 100% relief with the temporary one used for the trial. Any suggestions?
Deborah, the surgeon seems to suggest you that the skin need to heel first. So, massage, injections, TENS and other things that can irritate the skin may not be optimal for now. Repeated steroid injections can permanently weaken the tendons and thin the skin, so you may want to limit/avoid them in the future if possible.
There are several types of coccyx surgery (partial or complete removal, readjustment…). Ask the surgeon for the exact type of injury you have (fracture, dislocation…) and then you can ask this or some other coccyx surgeon about the optimal treatment. Note, that the coccyx has its function – it attaches the ligaments of the pelvic bones and tendons of muscles. Coccyx removal can result in loose pelvic floor muscles and the issues associated with it…
You can try to avoid sitting, especially on soft surfaces or you can use special doughnut cushions.
Very helpfull .. Article
I Have have accident 2.5 tone metals bar crushed on lower abdominal .. After that my urenary bloder ruptured and pelvik bone and l4 l5 region illum scrum part undisplced fractured seen.
Pubik synthesis and blader operations done now .. 3 months left now I am face and anl region sitting pain still I am not able to Sit above symptoms abserving
I cont do MRI now because having implant SS rod in pelvik how to now pain coming anl region and tailbone please reply me .. CT scan
Imran, it is a doctor who can tell if your pain comes from the coccyx (tailbone). An X-ray or CT of the coccyx can be done to check if the coccyx is damaged.
I had a fall 2 wks after bladder repair.on a slab floor.broke tailbone .it’s Been 14 months. Cant walk with out.had 3 disc ,bulging disc repaired in may.can’t do normal stretches etc.bladder still having issues.since I fell.haven’t been able to walk on hard floir,drive ,nothing think tailbone removal option.don’t know one who has history here in moline area that has done it okay .any referrals welcome
Ut pain.my bladder isn’t healing still having issues. Figure total removal is option
Mary, you can search for “coccyx surgeon” in your area. Surgery is last resort, no need to push it before trying other options. A doctor will want to make an X-ray first to be able to tell what exactly it is.
I fell on coccyx lot of pain sitting standing now have cystitis can this cause this
Mrs Dixon, falling on the coccyx by itself should not cause infectious cystitis, but it might be involved in developing interstitial cystitis.
I have been suffering for 5 months now.. I can sit..laying in bed hurts..each Dr says it’s radiating pain from my L5-S1 bulged disk. I can understand that but when I sit and moved I can physically feel that coccyx bone popping..and it feels like it moves. Then the pain is horrible.. I can literally feel my coccyx bone potruding out. I feel my life on hold. Just daily rotating around my “butt pain”! When I talked to my neurologist about it he said. Oh that’s normal. I don’t understand it never did it before. There was no trauma, I sat for 8 weeks do to OATS procedure on my knee and I was on crutches. Besides being slightly over weight and long term sitting no explanation for the severe and now chronic pain. Hurts to sit, hurts to get up..so while I’m at my desk at work I stand and sway back and forth leaning on my desk.. I probably look like a freak..lol what should I do..who do I need to see.. this is becoming unbearable! Please help!
Kimberly, it’s not necessary that the bulging disc L5-S1 causes your pain. In this article, you can scroll down and check the picture “Dermatomes” and see that the coccyx area is innervated by the nerves S2, S3 and S4 rather than S1.
It is possible that your coccyx is bent in the way that causes pain, but a doctor who specializes in coccyx pain could evaluate that. You may want to give the bulging disc some time to heal and see if that was the cause. When sitting, you may want to use wedged cushions, but do not just use some soft pads, which can make coccyx pain worse.
I fell off a ladder and hurt my tailbone. The pain went away but I am having burning and zapping like pain in my feet. Was wondering if this can be related to hurting my tailbone?
Janette, yes it can be. I suggest you to visit a neurologist or orthopedist.
I noticed that I get the tailbone pain from sitting too long on my sofa chair. Sitting or lying in my bed is much more comfortable and I rarely get pain from that. I think sofa chairs should be made with good springs and a little longer with a place to put your feet up to distribute the weight. This might help to not get this pain.
Zvezdana, when sitting on a semi-soft surfaces, like sofa chair, your bottom sinks into a chair, and your coccyx bends a bit, which can cause pain. A softer surface, like bed probably does not cause so much pressure. When sitting on a hard chair, the bottom and coccyx do not sink into the chair and can cause less pain than a soft chair.
I had fallen down steps3steps to the bottom ground where I live. I was walking great then went to see a bone doc then my tailbone feel worst. After a 2 month apearancemy legs hurt hard to. Walk when I go to the bath room it hurt a10 from1 to 10 I take.percocet 7.5-32/and lyrica 75mg andclonazepan.2 mg they just do not help
Stanley, you can ask your doctor what is your exact diagnosis or, if you haven’t got one, ask if some investigation, like X-ray would show more. When you know what exactly is wrong you can get appropriate treatment.
My brother in law has not been able to walk for a year.after many test the drs suspect motor Nero disease.He was told he couldn’t have an MRI scan because he had a pacemaker.We have been phoning around private hospitals for spines and was told he can have an MRI scan because he has a special pacemaker.So back to all the drs and they have checked and yes he can.They have all said if they could do MrRI that could show more for them.Looking on the web site he to me seems to have something wrong with his spine after he had a fall a year ago.Reading all the other people’s complaints it could be possible he has the same.We are going to fight to the end because he looks so well facially.eating happy and with good conversation but he can’t stand .He has that terrible pain in the spine like a knife going in when he is sitting too long.Any way what ever the outcome you have to try.
Thank you for this excellent article. I came upon to look, because I’ve been having pain since I started having chiropractic adjustments. I recalled having hurt my coccys real bad when I accidentally sat on the handle of a couch very hard. It hurt a few days and then it was gone, now it is back after 6 years. I wonder if the chriopractic adjustment triggered it. Now the pain extends to my left buttocks, anus, scrotum and hurrts when I urinate. I don’t have it chronically, some days are better than the others. With the encouragement of the other’s experiences and the article I will have an xray.
Jacob, the symptoms in the areas you’ve mentioned can be caused by a damage of the pudendal nerve and possibly other nerves. An X-ray can show if your coccyx is bent/broken and if you maybe need a surgery. However, to find the exact cause of your other symptoms a neurological examination and testing may be needed. I cannot say if chiropractic has done any damage, but I do encourage you to have some tests before further treatment.
I have similar pain it used to come two or three times a month but now it’s non stop pinching,sharp stabbing pain,have a golf ball size knot on my spine and my tailbone is very swollen and also my left buttock…I fractured my tailbone giving birth and the two after that they said just did more damage…If I’m moving it bothers me but sitting down or bedtime I dread it cause I can feel my heartbeat in every sore spot on my body and my daughter has to help me out of bed In the morning and if I move the wrong way it shoots a sharp stopping pain and I have the numbness but can still feel the pain in my bones….Dr told me it was a UTI and muscles in my lower back were just a little inflamed.But this is not stopping I feel like I’m in back labor 24/7 and I don’t know what to do .please help me!,,
Rebecca, I suggest you to see a doctor whom you trust to get a reliable diagnosis. A broken tailbone can be a cause of ongoing pain, but a doctor has to find out is your tailbone broken or not. A golf size bump does not like appear from an UTI.
Sir I got hurt while playing football 3 weeks back and pain started in my tailbone area. After that i thought it to be a normal pain and played for some more days. After some days I was not able to do anything. I went to doctors but they are not able to get anything. Now I am not able to bend forward or run even a little. Sometimes it pains even while walking or sitting or lying down. What should I do and from when can I resume running. Please help
Vishwesh, first, a doctor should be able to give you a diagnosis: does the pain arises from your coccyx or from muscles, etc. Physical examination and maybe an X-ray would be needed.
in agony. Broke Coxyc dec 2015 still in pain around my bottom and on coxyc area. How much longer? I fell on a hard floor in Doctors Surgery. I want to go back to work help no Xray given
Carol, one option is a surgical coccyx removal, but research this option and discuss with a reliable surgeon before undergoing surgery.
I’ve had pain in my tailbone for 30 years + . It started when a lad at school pulled a chair away as I was about to sit . The pain was awful . I’ve suffered with back pain, hip pain and pain in my buttocks for years since on and off .
I have infused L4-L5, L5-S1 disc of 3 mm…. I experienced awful pregnancy pain from 6 mths and on with pain radiating from pelvic area, low back pain, sacrum area, and my knees would go out on me while walking so i would fall on my knees. I had seen a chiropractor and a physical therapist for the remainder of my pregnancy. I experienced so much excruciating pain in the pelvic area and the sacrum are when i had to get up from a chair, or simply to roll over from side to side in bed, and trying to get up each morning was so painful i would dreadfully force myself out of bed in tears. In the end it was all worth it having delivered a healthy, BIG baby girl of 8.8LBs. I am only 5 ft and weigh 100 LBs so my Baby definitely took a toll on my body. 1 mth after delivery, my pains got so worse that i couldn’t walk anymore. Had MRI done and learned that i had a stress fracture on my LT Sacrum and now my discs were out to 5.5mm. I’ve had 3 Epidural steroid shots at L5-S1 area which seemed to work wonderfully in relieving pain!…. That was 4 yrs ago. Well i had my 2nd girl last December, another big one at 7.13 LBs, and almost identically went thru the same debilitating process again….. A month after delivery i no longer could walk with excrutiating pain on my low back and Tail bone area……. since my delivery in December 2014, i now have had 5 Epidural steroid injections. MRI shows no fracture. However, i have an inch of tail bone that sticks out and is so painful. Instead of last digits of tailbone curving inward, it protrudes so much that it touches the wall every time i lean against a wall. Help!!!!! Since my pain initiated thru pregnancy, i can’t find a specialist who has experience with this types of pain to help me!….13 mths since i delivered my 2nd baby and it’s not getting any better. Can removing coccyx help my condition?
Angela, I think, first, you need to give your body some time to re-adjust to your nonpregnant form. You mentioned a bulging disc, stress fracture and coccyx that sticks out. I mention other causes above in the article. So your pain my originate from various sites, not only from coccyx.
There are doctors tat specialize in coccyx pain – they are usually orthopedists; you might be able to contact someone online. Coccyx removal can help, but only in specific cases, a specialist can tell and can differ from person to person.
Make a detailed but compact list of all of your symptoms as you experienced them, where exactly did you feel pain and what were exact pain triggers and relievers and find a good orthopedist to discuss with.
I need to speak to some that have had their coccyx removed. I’m 6 months post op and have had so many complications. I’m now dealing with major swelling on my right side all the way down my leg. I’m still unable to sit. I had my surgery done my a Duke orthopedic surgeon. Please anyone that has has this surgery contact me. Thank you
Cindy, it’s unlikely many people with coccyx surgery will appear here. You may want to try on some big health forum like medhelp.org or healthboards.com or you can check coccyx.org and try to contact the author who apparently knows quite some doctors who may be able to advise you.
Just wanted to say thanks for this comprehensive summary. Most of the typical sources for the public are very minimal and do not offer not very useful information (e.g. they tend to recommend “donut” cushions).
Dynamic X-rays are not an option for most people, that might be noted. I experienced a clear trauma that saw me in the hospital. They didn’t bother with X rays. GP I saw a week later did order them.
I tried to politely ask the tech about a dynamic X-ray, and they were offended that I asked, took it as a suggestion they didn’t know what they’re doing. The radiologist in the adjacent room also thought this request was out of line.
They took three views with me lying down. The front was bound to be junk due to the coccyx being obscured by organs etc, the tech even told me that. The back- I’ve read that they often miss the actual coccyx, not sure if it happened in this case. The lateral view they did take was of the side on which I *don’t* have pain. I mentioned this, didn’t matter. Now I have a negative X-ray, and that’s it. My GP is just going to look at that report.
My pain while lying down or standing less than it was when this happened a few weeks ago, but I have pain *walking*, past mid-stride. I don’t know who I can see to help with that but am not hopeful anyone will either know what to do or be able to help.
Karie, they are orthopedists that specialize or have experience with treating coccyx pain. Obviously, you can’t expect that this will be solved between your GP and radiologists…
Thanks, Jan. I *don’t* expect my GP to manage this. The issue is that where I live, in my health care system, I wouldn’t be able to see an orthopedist without a referral from my GP. My GP doesn’t know a lot about ortho issues in general, and always defers to whatever reports from radiology. Getting a second opinion from another GP would be the logical next step in this case, except that they’re in short supply in my area, and you have to leave your GP’s practice in order to be eligible for consideration to enter a new one. There are waiting lists. Etc.
Karie, your GP may be doing what he believes is right, but it’s you who need to decide if you trust him or not. What you can do is to actually write down a detailed list of your symptoms, where exactly do you feel pain, where does it radiate, is there any numbness or tingling or any other symptoms, what are triggers and relievers, including certain body positions, etc…This will make you more confident when discussing with doctors. You didn’t say what injury you had and where do you feel pain. Two examples of causes of lower back/buttock pain not related to coccyx are a herniated disc in the lumbar spine and piriformis syndrome.
I experienced a blunt trauma to my tailbone, the force of which caused immediate pain, just to that area (as well as nausea; I also fainted [but did not experience head trauma or injury elsewhere). The pain is very localized, to the bottom of my tailbone, on the left side. Fortunately, I have no other symptoms, such as tingling down the legs.
The problem, as far as I’m concerned, is not so much about communication – I am clear and polite, at least that’s always my intention.
As far as I’m concerned, the issue is more that he will simply ignore his own initial clinical assessment if it is not clearly backed up by a report. (For example, two X-rays were taken a few years apart to evaluate whether or not I had arthritis [the second was also for an injury in that location]. He just went along with the most recent X-ray finding and didn’t question the inconsistency. There have been a couple of other soft tissue injuries in which reports were unclear or negative; a physiotherapist made a diagnosis where my GP did not.)
So I don’t trust him for MSK issues at all, based on past experience. I’d go to my physiotherapist, except she can’t order the imaging.
I think in some ways it might be a moot point, as I understand that there’s whether it’s a fracture or a bruise or whatever, the treatment is the same (rest and pain management).
The thing that concerns me is the pain during walking. This seems to be less usual than pain during sitting, for a coccyx injury, from what I have read.
I agree that I will have to decide what to do about my GP – it’s just that leaving is not so easy, because there’s no guarantee I’ll find another soon.
Thank you for your help, and again for this site – it is really the most comprehensive I have seen.
Best,
Karie
In any case, thank you for the conversation.
Karie, as you may know, X-ray cannot show a bone bruise, neither can CT, only MRI can. Pain from bone bruise lasting for 2 years would be theoretically possible, but I’m not trying to suggest you this is your problem or that you should have MRI. If the pain is slightly to the left, then maybe a ligament or nerve could be involved…I don’t know what to say. One surprising thing is that sitting on soft chairs can cause pain even in healthy coccyx.
November 25, 2015
I’ve been miserable going on 7 years now. I’ve had multiple spine surgeries, the last 10 months ago where I had total spine reconstruction. I received a diagnosis about 5 years ago being PNE, Pudendal Nerve Entrapment.
The pain starts in the left side of the rectum. It’s a burning pain that extends into my buttocks, left testicle, and predominately the left side of my penis. Sitting in both hard and soft chairs and lifting exacerbates the pain. Eventually I become nauseous if nothing is done to try and get relief.
The most comfortable seat I have in the house is my toilet seat. I get immediate relief when there. I’ve been using a hemoroid donut for the last 6-7 years and it helps make life bearable. It does get quite embarraing carrying this into public places like restaurants, Church, and sports events. My wife thinks I hate her but to date has not complained about the reduction in size of my penis. I’m not able to attain a full erection.
I’m very dependent on opioids pain medications. Non opioids don’t even come near giving any relief necessary to try and attain normal living.
I’ve had 40-50 injections over the years with varying degrees of “temporary relief”. They are not long term solutions for anyone but might postpone surgery if needed. The longest I’ve felt relief has been about 90 days.
I return for follow up with my surgeon, Dr Isadore Lieberman, in Dallas, Tx this coming January. I’m researching surgery to have my Coccyx removed and best I can tell this may be my best option. He is very capable and I highly recommend him to anyone who suffers spine problems.
My advice to men are to not be bashful about discussing these intimate problems you suffer with medical professionals. They are best equipped to get you help if they know all the details. It’s best if you journal your pain. Least over a 10 day period to let them know when, where, and why the pain flares up.
I’ll try to post a follow up after my next procedure as to the outcome. I wouldn’t wish this pain on my worst enemies.
God Bless and Good Luck,
Jim Clanton
jim, coccyx removal has its own downsides, so I hope you can discuss this with your doctor thoroughly.
I fell in 2012 and fractured my sacrum. My pain is non stop. I’ve tried accupuncture..chiropractic..epidural…two illiac joint injections…steroid injections in the tailbone…no relief from any of those procedures. Now they want to remove it. However..recovery from such a surgery can be up to two years!!! I’ve suffered 3 years already. Not so sure that is the answer.
Barbar, surgical correction, not only removal, might be possible. Try to discuss this with a surgeon who has experience with coccyx.
My fiance have been drinking coxflam for 10years. She gets pain and mucle tention reggularly. Xrays shows nothing. What can it be and how can it be treated it is obviously not good drinking painkillers costantly.thanks
bianca, I don’t know what is the cause of her pain and why she is taking coxflam. If it is a physical problem, an orthopedist or neurologist can help. If it is a personal or psychological problem, a good wise friend or counselor can help.
I fell twice on my coccyx 4 hrs ago had xrays MRI showing nothing the pain was agonising then I heard about Michael Durtnall sayer clinic London he x rayed me standing and it clearly showed a dislocation of my coccyx it was such a relief to finally have someone who believed me I’ve had a few sessions and already I’m fifty per cent better and Michael has assured me he can get it 90 per cent better.
Hello. I have adult scoliosis and have had two lumbar surgeries (with titanium screws to strengthen my spine). The 2nd surgery (August, 2014), was supposed to relieve my sciatica, but seemed to move it elsewhere. I still have the sciatica but also now have coccyx pain all the time, when sitting, walking, going up and down stairs — almost anything physical. My Orthopaedic dr. says that having the coccyx removed will help but I fear having it done because this same dr. said that fusion of L 4, 5 and S1 would relieve my sciatica which DID NOT get corrected, so why should I believe that removal of the tailbone will help? I’m so frustrated! Can anyone give me advice, please?
Dana, coccyx removal can help to relieve pain if the origin of pain is actually in the coccyx. Note that coccyx removal has its own downsides (read above in the article). If you think you cannot trust your doctor, ask for a second opinion.
Sir I am a cricketer and in cricket I do bawling…Sir my first weight was 70 and now 83.when I bawling a pain produce in my backside attached at lift side at ending of backbone but now an another pain produce at the ending of backbone and some oily liguid releases continue when I touch it I feel a little injury just in the end of backbone.Sir what is the cause and treatment of this. My age is 22.
Bilal,
I don’t know what it is, but it could be pilonidal cyst (there is a short description above in the article, but you can also search on internet), or an abscess (a collection of pus) due to a skin injury. I strongly suggest you to check this with a doctor. I can’t recommend any remedies; a doctor should know what kind of treatment you need.
I have awful tailbone ache that wakes me laying on my back, but not when sitting or touching the bone. I lost a lot of weight (lowering steroids for Lupus w. DM) but was thin most of my life and never felt my tailbone protrude. Now it feels like an inch wide round stone that extends into each side of buttock mid-way (if lying opposite side) Still 25 lbs over ideal weight, but feel the tailbone as a large painful lump after back sleeping on a soft mattress at incline for reflux and chronic fractures at T9-10 (hard mattress worse for that). Since bone growths are visible in my jaw (thought benign by dentist), I’ve wondered if it is enlarged? How large should the tailbone top be in a 5foot 2 inch small frame,.and wouldn’t I have felt it back when I was 30 lbs thinner if it was large then (some years ago)? Is it likely to be cancerous/enlarged?
I have been suffering from tailbone pain for 4 years. It came on suddenly, no trama. I had an MRI, bone scan and did PT with no relief. Finally had a cortisone injection and it felt 100% better until the birth of my first and after 5 days in a hospital bed sitting awkwardly, the pain returned. I suffer every day, some days worse than others. My husband suffers to while having to listen to me complain and watch me be uncomfortable everywhere, couch, car, bed, restaurants… I have found ways to compensate for the pain and feel as though I am doing damage to other parts of my body because of it. Not sure where to go from here. I am 29, with two young children and hate suffering from this pain that every doctor dismisses.
Delivery can break or dislocate the tailbone, so your situation may not be the same as when you have the initial imaging tests. Another injection can help again and you can discuss with your doctor about another MRI.
Ask your dr for another shot. Sometimes the shots can last a whole year and even longer. You can get 3 shots in a 12 month span. If you found relief the first time you should do it. I have an appointment in 2 weeks for another round in my neck. The original shot has lasted almost 2 years for me.
MRI done 5 months after a fall shows contusion fractures of two of coccyx vertebrae. Living on opioid pain meds and getting no pain relief. Just stupor. Can’t sit, walk or enjoy normal life at all. Often have to use a walker, especially in morning. Will try to get Pain Specialist to inject steroids as radiologist states there is significant edema around the site – all these months later. Now, having pelvic pain as well. Each day is worse than the next. Life is unbearable. Any suggestions?
Cathy, partial or complete surgical coccyx removal is one option to discuss with an orthopedist. The effectiveness of a surgery greatly depends on circumstances as you can read above in the article. Surgery is often successful when coccyx pain is due to trauma.
This website helped me understand what to do. I am going to get my mum to book an x-ray as some of the symptoms i am having are under the fracture column. I have been taking ibuprofen and now i know its ok.
Thanks alot
I hve tail bone pain nd since that I hvng vaginal and hip pain also I don’t know why I am having pain in other regions also and I hve multiple sclerosis also please hlp me
Riya, you may want to see a doctor.